2025 October 15;6(10):1440-1443. doi: 10.37871/jbres2200.
Cis-platin Plus Paclitaxel Treatment in Cervical Carcinoma induce Hyperthyroidism: A Case Report
Ashanjiang Aniwan*, Jian Mei, Xiaoye Deng, Guangli Ding, Hongli Zhou and Bichao Yu
Abstract
A patient in their 70s with cervical carcinoma developed hyperthyroidism after receiving treatment with cisplatin and paclitaxel. Laboratory tests confirmed the patient’s hyperthyroid status. Following the administration of anti-thyroid medications and the completion of the chemotherapy regimen, the patient’s thyroid function tended to stabilize. This case is infrequent, as few prior associations have been reported between these specific chemotherapeutic agents (cisplatin and paclitaxel) and hyperthyroidism. It thus suggests the existence of potential pathophysiological mechanisms underlying this phenomenon, underscoring the necessity of conducting further in-depth investigations. It also serves as a reminder to clinical practitioners that when encountering patients receiving chemotherapy who present with such symptoms, clinicians should consider hyperthyroidism in the differential diagnosis.
Background
Hyperthyroidism is a condition in which the thyroid gland produces an excessive amount of thyroid hormones [1]. Include autoimmune disorder, thyroiditis, and certain medications or supplements.
Chemotherapy, as a systemic therapy, is one of the most effective modalities for cancer treatment. Cisplatin and paclitaxel are commonly used in the treatment of various cancers, especially cervical cancer, ovarian cancer, lung cancer. They are often used in combination due to their synergistic effects in inhibiting cancer cell growth [2,3]. The direct mechanism is Cisplatin primarily acts by cross-linking DNA, leading to DNA damage and cell death [4]. Paclitaxel works by stabilizing microtubules and disrupting cell division [5]. However, there is no known specific interaction between these drugs and thyroid cells or the pathways involved in thyroid hormone synthesis (iodine uptake, oxidation, and organification), release, or regulation by the hypothalamic-pituitary-thyroid axis [6].
The known pharmacological actions and side effect profiles of cisplatin and paclitaxel haven’t include any direct or specific effects on the thyroid gland yet [7-9].
In this paper, we report a patient who developed hyperthyroidism after receiving cisplatin plus paclitaxel treatment for cervical carcinoma.
Case Presentation
A patient in their 70s, previously diagnosed with cervical cancer, was referred to our clinic with hyperthyroidism following chemotherapy. The patient had received a chemotherapeutic regimen consisting of cisplatin (70 mg on Day 1) and paclitaxel (270 mg on Day 1). After each chemotherapy session (four session in total), the patient frequently experienced severe tachycardia, often accompanied by feelings of anxiety. Marked hand tremors and significant involuntary weight loss were also observed; however, these symptoms were initially attributed to chemotherapy-related side effects.
Laboratory tests confirmed hyperthyroidism 2 months after first cycle of chemotherapy, and a timeline was used to illustrate the patient’s clinical changes (Figure 1). Clinical observations and laboratory investigations were conducted during and after the first two cycles of chemotherapy. Following the third cycle, the patient’s aforementioned symptoms exacerbated, prompting hospital admission to our clinic. TSH (Thyroid Stimulating Hormone) receptor antibody (TRAb) test and thyroid technetium scintigraphy (ECT) was performed, which yielded negative results with TRAb < 0.82 IU/L and ECT shows normal technetium uptake function. Based on clinical judgment, treatment with anti-thyroid medication was initiated at a dosage of methimazole (Thiamazole) 20 mg once daily (qd) via oral administration (po).
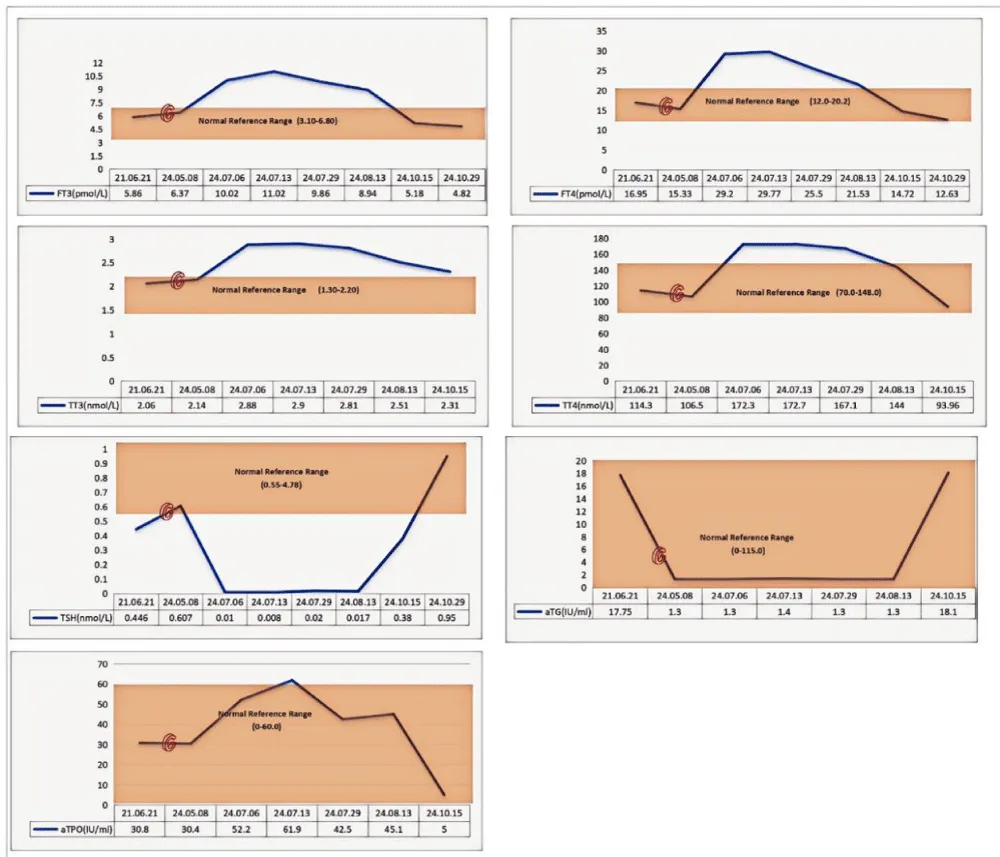
With continued anti-thyroid treatment and completion of the chemotherapy regimen, the patient’s condition improved. The dosage of methimazole was gradually tapered, and subsequent thyroid function tests were performed. A follow-up thyroid ECT was conducted 3 months after treatment initiation; this test also returned negative, and laboratory examinations revealed that the patient’s thyroid function tended to stabilize. Ultimately, we summarized a comparison of thyroid function indicators before and after chemotherapy, as well as during anti-thyroid treatment (Figure 2). These findings suggest a potential association between cisplatin/paclitaxel-based chemotherapy and the development of hyperthyroidism in this patient.
Conclusion
In this case report, we describe a patient who developed hyperthyroidism following chemotherapy with cisplatin and paclitaxel for cervical cancer. While this clinical scenario is extremely rare, there is a paucity of prior reports directly linking these two chemotherapeutic agents to hyperthyroidism.
Furthermore, several other chemotherapy drugs have been associated with thyroid dysfunction. For instance, immune checkpoint inhibitors (e.g., pembrolizumab and nivolumab) may disrupt thyroid function, potentially leading to hyperthyroidism [10]. Additionally, certain cytotoxic agents and targeted therapies carry the risk of inducing hyperthyroidism, though the specific manifestations vary depending on individual patient differences and the unique mechanisms of action of these drugs.
These observations provide a framework for exploring how cisplatin and paclitaxel might contribute to hyperthyroidism. Similar to other cytotoxic drugs [11-12], cisplatin may exert direct effects on thyroid follicular cells, potentially impairing cell membrane integrity, disrupting organelle function, and interfering with the normal synthesis and secretion of thyroid hormones. Moreover, cisplatin may modulate immune and hormonal regulatory pathways within the thyroid microenvironment. Overall, this case underscores the complexity of chemotherapy-induced hyperthyroidism and emphasizes the need for further research to better understand and manage this rare yet clinically significant complication.
A key clinical message of this manuscript merits greater emphasis to maximize its relevance for clinical practice: when managing patients undergoing the chemotherapy regimen, clinicians should proactively incorporate hyperthyroidism into their differential diagnosis if the patients present with relevant manifestations-specifically, symptoms such as unexplained tachycardia, persistent anxiety, marked hand tremors, or involuntary weight loss. These symptoms are often initially attributed to chemotherapy-related side effects, as observed in this patient’s initial clinical course; thus, explicitly highlighting the need to consider hyperthyroidism in such scenarios will not only draw attention to this underrecognized complication but also substantially enhance the clinical impact and educational significance of this case report. By underscoring this diagnostic consideration, the manuscript can better serve as a practical reminder for frontline clinicians, aiding in the timely identification and management of chemotherapy-induced hyperthyroidism to improve patient outcomes.
References
- Elbe H. Once upon a time in Anatolia: the kings with bulging eyes. Hormones (Athens). 2024 Dec;23(4):841-847. doi: 10.1007/s42000-024-00561-y. Epub 2024 Apr 18. PMID: 38632215.
- Nasioudis D, Pashankar FD. Management of recurrent and persistent malignant ovarian germ cell tumors: a narrative review. Int J Gynecol Cancer. 2024 Sep 2;34(9):1454-1460. doi: 10.1136/ijgc-2023-005052. PMID: 38991656.
- Yang ST, Wang PH, Liu HH, Chang CW, Chang WH, Lee WL. Cervical cancer: Part II the landscape of treatment for persistent, recurrent and metastatic diseases (I). Taiwan J Obstet Gynecol. 2024 Sep;63(5):637-650. doi: 10.1016/j.tjog.2024.08.001. PMID: 39266144.
- Elmorsy EA, Saber S, Hamad RS, Abdel-Reheim MA, El-Kott AF, AlShehri MA, Morsy K, Salama SA, Youssef ME. Advances in understanding cisplatin-induced toxicity: Molecular mechanisms and protective strategies. Eur J Pharm Sci. 2024 Dec 1;203:106939. doi: 10.1016/j.ejps.2024.106939. Epub 2024 Oct 17. PMID: 39423903.
- Drugs and Lactation Database (LactMed®) [Internet]. Bethesda (MD): National Institute of Child Health and Human Development; 2006–. Paclitaxel. 2024 Jan 15. PMID: 29999636.
- Hamnvik OP, Larsen PR, Marqusee E. Thyroid dysfunction from antineoplastic agents. J Natl Cancer Inst. 2011 Nov 2;103(21):1572-87. doi: 10.1093/jnci/djr373. Epub 2011 Oct 18. PMID: 22010182; PMCID: PMC3206040.
- Sousa-Pimenta M, Estevinho LM, Szopa A, Basit M, Khan K, Armaghan M, Ibrayeva M, Sönmez Gürer E, Calina D, Hano C, Sharifi-Rad J. Chemotherapeutic properties and side-effects associated with the clinical practice of terpene alkaloids: paclitaxel, docetaxel, and cabazitaxel. Front Pharmacol. 2023 May 9;14:1157306. doi: 10.3389/fphar.2023.1157306. PMID: 37229270; PMCID: PMC10203197.
- Adhikari S, Nath P, Das A, Datta A, Baildya N, Duttaroy AK, Pathak S. A review on metal complexes and its anti-cancer activities: Recent updates from in vivo studies. Biomed Pharmacother. 2024 Feb;171:116211. doi: 10.1016/j.biopha.2024.116211. Epub 2024 Jan 29. PMID: 38290253.
- Zraik IM, Heß-Busch Y. Management von Nebenwirkungen der Chemotherapie und deren Langzeitfolgen [Management of chemotherapy side effects and their long-term sequelae]. Urologe A. 2021 Jul;60(7):862-871. German. doi: 10.1007/s00120-021-01569-7. Epub 2021 Jun 29. PMID: 34185118.
- Hansen JF, Magyari M, Rasmussen ÅK, Sellebjerg F, Feldt-Rasmussen U. Alemtuzumab-induced thyroid disease: A Danish cohort study. Mult Scler Relat Disord. 2024 Nov;91:105880. doi: 10.1016/j.msard.2024.105880. Epub 2024 Sep 6. PMID: 39293122.
- Kumar L, Upadhyay A, Jayaraj AS. Chemotherapy and immune check point inhibitors in the management of cervical cancer. Curr Probl Cancer. 2022 Dec;46(6):100900. doi: 10.1016/j.currproblcancer.2022.100900. Epub 2022 Oct 11. PMID: 36265252.
- Sahara S, Herzog AE, Nör JE. Systemic therapies for salivary gland adenoid cystic carcinoma. Am J Cancer Res. 2021 Sep 15;11(9):4092-4110. PMID: 34659878; PMCID: PMC8493384.
Content Alerts
SignUp to our
Content alerts.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.