> Medicine Group. 2021 May 12;2(5):320-322. doi: 10.37871/jbres1234.
Pneumatocele in COVID-19 Infection: A Harbor of Future Complications
Aqusa Zahid, Mohammad Yaseen and Naveed Rashid*
- Pneumatocele
- COVID-19
- Pneumothorax
Abstract
The year 2020 has been marked by the pandemic caused by severe acute respiratory syndrome coronavirus 2(SARS CO-V-2) disease (COVID-19). The virus has infected millions of people around the world. Lung is the most commonly affected organ of body. Various radio-logical manifestation of disease on lungs reported so far include ground glass, consolidations. Cysts or pneumatocele have rarely been reported. We here present a case of patient who presented to us with a spontaneous pneumothorax and during surgery was found to have pneumatocele. The aim of the case here is to highlight the variety of ways COVID-19 can affect the lungs.
Introduction
COVID-19 virus pandemic has swept the world rapidly. With every passing day a new aspect of its effect on human body unfolds. Lung is the most common and most severely affected organ of human body by the virus. Viral infection causes symptoms from mild upper respiratory tract infection to severe acute respiratory distress syndrome needing mechanical ventilation [1]. Studies on radiologic features of COVID-19 have reported various features like ground glass, consolidations, and cyst [2]. Pneumatoceles are rarely reported in COVID-19 infection. With this case we highlight an important radiological manifestation of the disease and how this can lead to development of pneumothorax.
Case Report
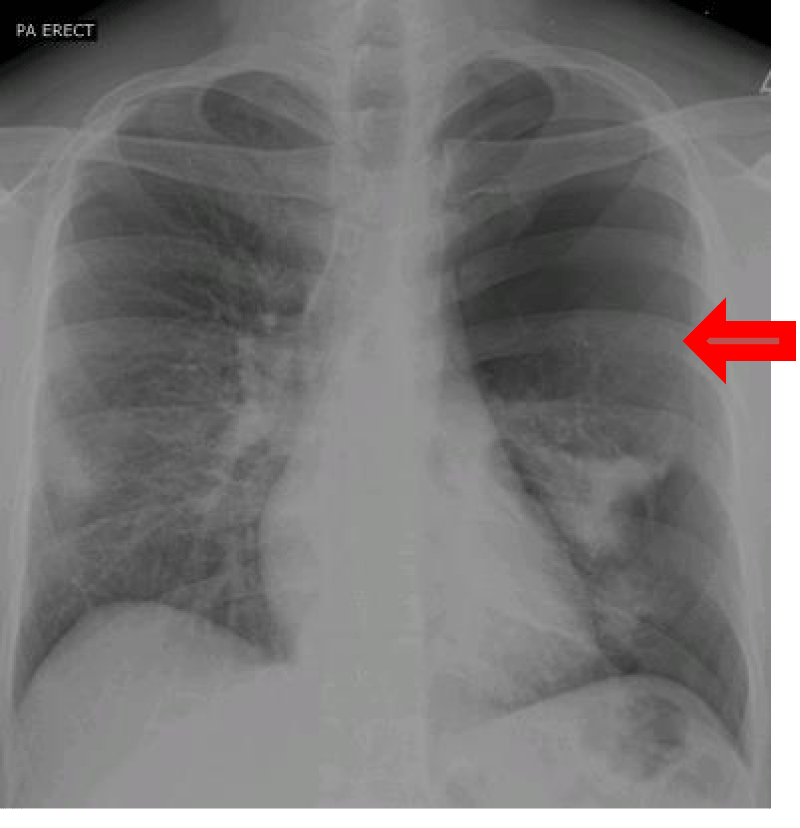
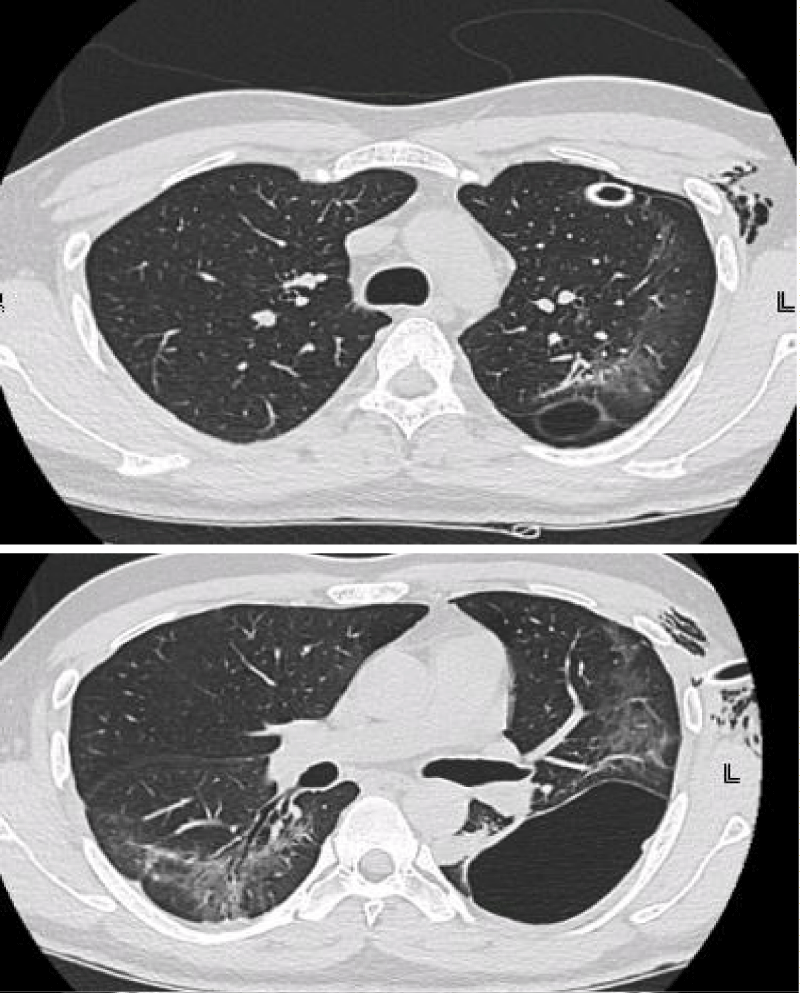
A 34-year-old male before presentation to us had acute history of cough and fever. He tested positive for covid-19 on RT-PCR and since the patient was stable, he was managed conservatively with symptomatic care and kept in isolation for 15 days. The patient developed sudden onset left sided chest pain and cough, 5 days after discontinuation of isolation. So he rushed to emergency services. On presentation to the emergency services the patient was tachycardic and tachypneic while hemodynamically stable maintaining oxygen saturations more than 90% on breathing room air. Chest examination revealed absent breath sounds on left side with hyper resonant percussion note. An urgent chest X-ray (Figure 1) was done which showed large left sided pneumothorax. Tube thoracostomy was perfomed, and patient was shifted to ward. Patient remained clinically stable. Air leaked persisted after 72 hours of tube thoracostomy so a CT scan chest was performed which showed mild residual pneumothorax and a large thin-walled cystic lesion in the left lower lobe adjacent to the pleural surface (Figure 2).
Thoracic surgery was consulted and patient was planned for video assisted thoracostomy (VATS).
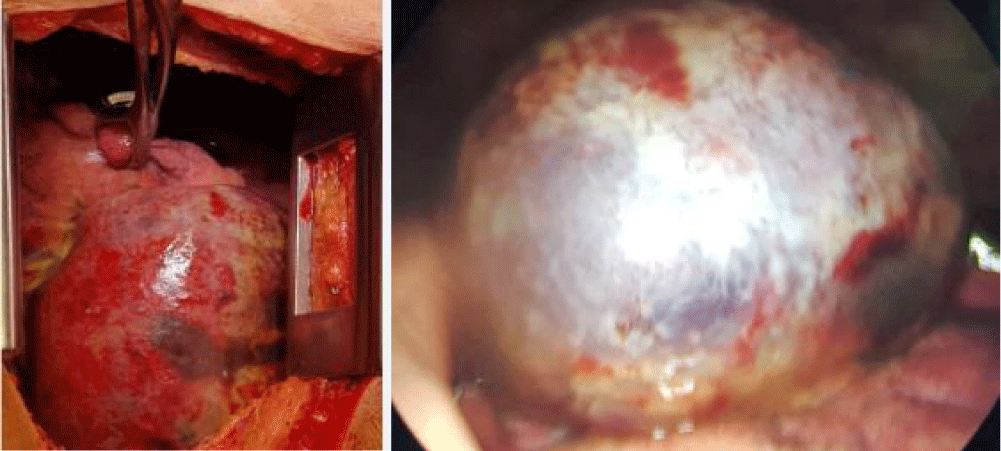
VATS showed a large left sided pneumatocele involving the left lower lobe superior segment (Figure 3). Considering the large size of pneumatocele VATS was abandoned and thoracotomy was performed.
Pneumatocele was resected and over sewn. Mechanical pleurodesis was also performed and two chest tubes were kept in place. The patient improved clinically and was discharged home.
Discussion
Pneumothorax is now a well reported complication of COVID-19 infection. The incidence of pneumothorax in COVID infection is reported to range from 0.6-1% [3]. Positive pressure ventilation and ARDS increases the risk of development of pneumothorax as identified in a number of case series, our patient did not have any of these risk factors [4]. Another important risk factor identified is prolonged coughing [5]. The hypothesis towards development of spontaneous pneumothorax and pneumomediastinum in COVID-19 is that the virus affects peripheral and subpleural regions of the lungs and progressive inflammation in these parts leads to development of cysts or pneumatocele rupture of these later on may present as pneumothorax pneumomediastinum or sub cutaneous emphysema [6]. Baseline imaging may predict development of pneumothorax in patients with COVID-19. More over a case series identified patients who had raised inflammatory markers were at increased risk of developing pneumothorax [7]. Detailed evaluation of more of such cases will help understand the mechanism of pneumothorax further.
Authors’ Contributions
AZ has made contributions in drafting the manuscript and revising it critically for important intellectual content.
NR was primary physician and has made contributions in drafting the manuscript and revising it critically for important intellectual content.
MY has made contributions in drafting the manuscript and revising it critically for important intellectual content.
All authors read and approved the final manuscript.
Informed Consent
Obtained from the patient.
References
- Zhao D, Yao F, Wang L, Zheng L, Gao Y, Ye J, Guo F, Zhao H, Gao R. A Comparative Study on the Clinical Features of Coronavirus 2019 (COVID-19) Pneumonia With Other Pneumonias. Clin Infect Dis. 2020 Jul 28;71(15):756-761. doi: 10.1093/cid/ciaa247. PMID: 32161968; PMCID: PMC7108162.
- Ng MY, Lee EYP, Yang J, Yang F, Li X, Wang H, Lui MM, Lo CS, Leung B, Khong PL, Hui CK, Yuen KY, Kuo MD. Imaging Profile of the COVID-19 Infection: Radiologic Findings and Literature Review. Radiol Cardiothorac Imaging. 2020 Feb 13;2(1):e200034. doi: 10.1148/ryct.2020200034. PMID: 33778547; PMCID: PMC7233595.
- Zantah M, Dominguez Castillo E, Townsend R, Dikengil F, Criner GJ. Pneumothorax in COVID-19 disease- incidence and clinical characteristics. Respir Res. 2020 Sep 16;21(1):236. doi: 10.1186/s12931-020-01504-y. PMID: 32938445; PMCID: PMC7492794.
- Brahmbhatt N, Tamimi O, Ellison H, Katta S, Youssef J, Cortes C, Gotur D. Pneumatocele and cysts in a patient with severe acute respiratory syndrome coronavirus 2 infection. JTCVS Tech. 2020 Dec;4:353-355. doi: 10.1016/j.xjtc.2020.08.047. Epub 2020 Aug 21. PMID: 32864633; PMCID: PMC7441992.
- Brahmbhatt N, Tamimi O, Ellison H, Katta S, Youssef J, Cortes C, Gotur D. Pneumatocele and cysts in a patient with severe acute respiratory syndrome coronavirus 2 infection. JTCVS Tech. 2020 Dec;4:353-355. doi: 10.1016/j.xjtc.2020.08.047. Epub 2020 Aug 21. PMID: 32864633; PMCID: PMC7441992.
- Shah V, Brill K, Dhingra G, Kannan S. Delayed recurrent spontaneous pneumothorax in a patient recovering from COVID-19 pneumonia. Korean J Anesthesiol. 2021 Apr;74(2):183-185. doi: 10.4097/kja.20400. Epub 2020 Sep 1. PMID: 32867010; PMCID: PMC8024203.
- Martinelli AW, Ingle T, Newman J, Nadeem I, Jackson K, Lane ND, Melhorn J, Davies HE, Rostron AJ, Adeni A, Conroy K, Woznitza N, Matson M, Brill SE, Murray J, Shah A, Naran R, Hare SS, Collas O, Bigham S, Spiro M, Huang MM, Iqbal B, Trenfield S, Ledot S, Desai S, Standing L, Babar J, Mahroof R, Smith I, Lee K, Tchrakian N, Uys S, Ricketts W, Patel ARC, Aujayeb A, Kokosi M, Wilkinson AJK, Marciniak SJ. COVID-19 and pneumothorax: a multicentre retrospective case series. Eur Respir J. 2020 Nov 19;56(5):2002697. doi: 10.1183/13993003.02697-2020. PMID: 32907891; PMCID: PMC7487269.
Content Alerts
SignUp to our
Content alerts.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.