Medicine Group. 2024 August 31;5(8):1067-1069. doi: 10.37871/jbres1990.
Unusual Cause of the Chest Pain: Oesophageal Lipoma
Jabali Fatima A1, Alganm Sara A1, Alrajhi Sulaiman M1, Alotaibi Tareq Z1, Alghamdi Abdulaziz A2 and Daghistani Rayyan A1*
2Thoracic surgery, Department of Surgery, King Abdulaziz Hospital, Ministry of National Guard Health Affairs, Alahsa, Saudi Arabia
Case Report
An 86-year-old woman with a history of multiple chronic conditions, including hypertension, diabetes, dyslipidemia, hypothyroidism, and glaucoma, presented to the family medicine clinic. She reported experiencing chest pain for the past two days. The pain was described as a pressure sensation, and she denied any dyspnea, shortness of breath, or paroxysmal nocturnal dyspnea. Upon examination, she appeared well and was vitally stable. Both the ECG and troponin levels were normal.
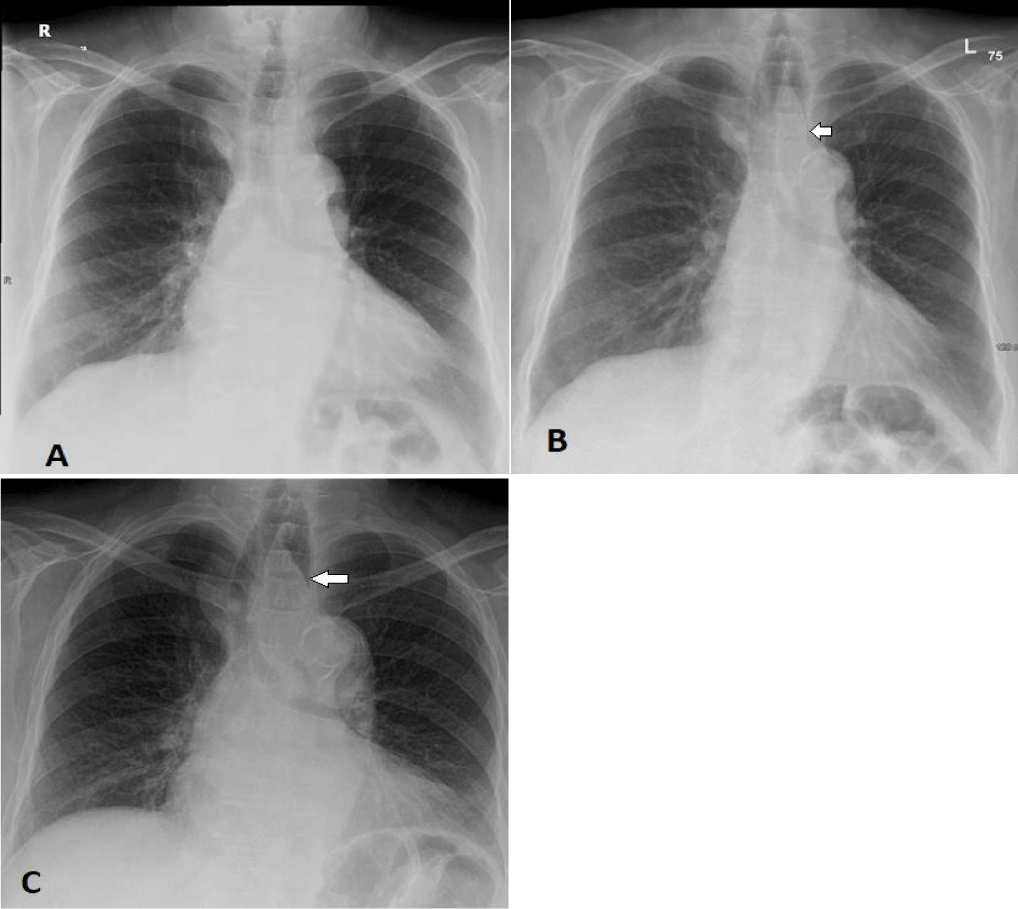
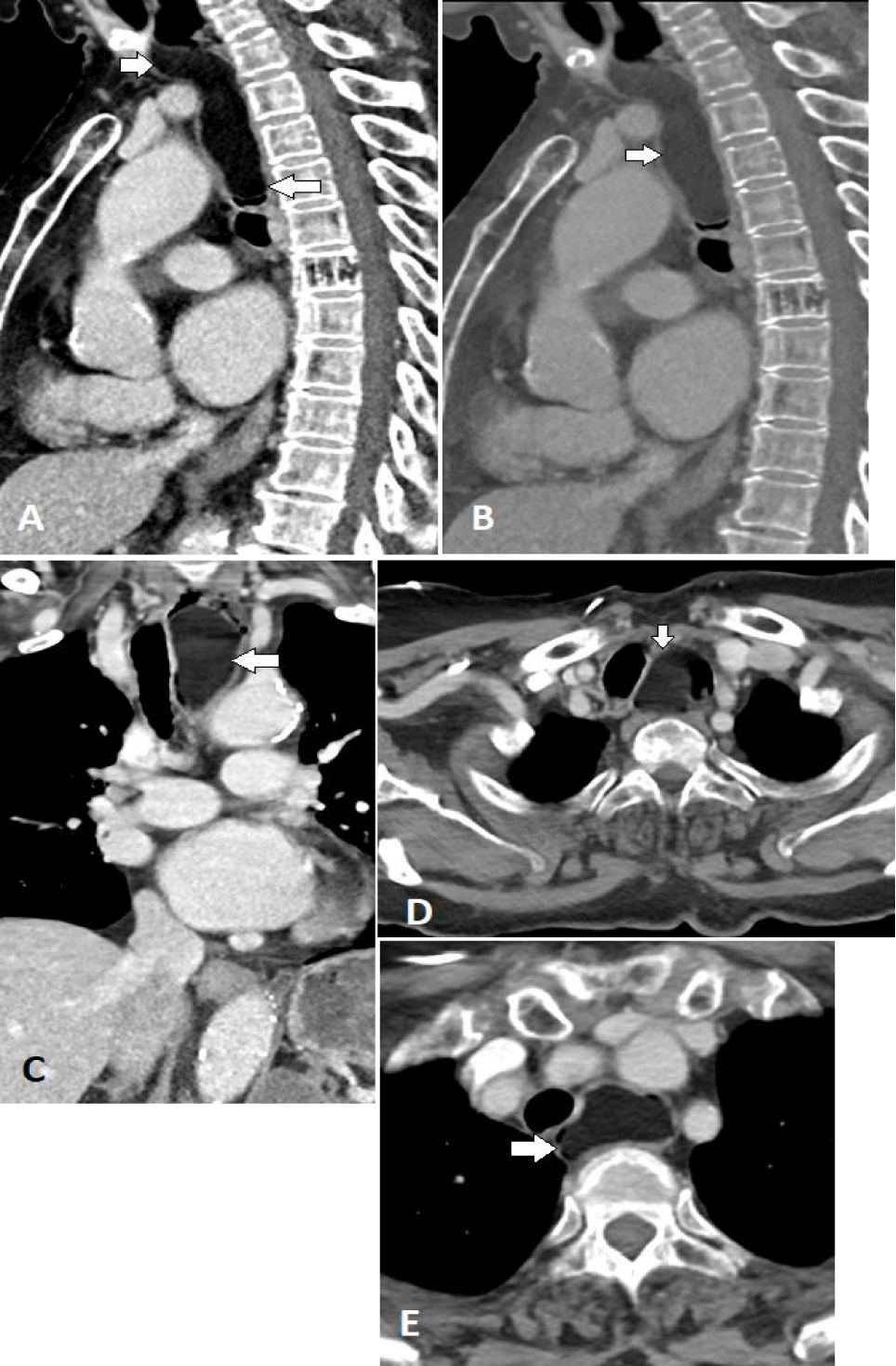
A chest X-ray (Figure1) revealed a soft tissue density in the middle mediastinal compartment, causing compression of the oesophageal column with smooth tapering. A further assessment by CT scan of the chest (Figure 2) identified a pedunculated, fat-density mass in the upper third of the oesophagus, resulting in obstruction and mild dilation of the proximal oesophagus, consistent with the lesion observed in the previous radiograph. No oesophageal thickening or abnormal enhancement was present, no soft tissue component and there was no enlargement of local lymph nodes.
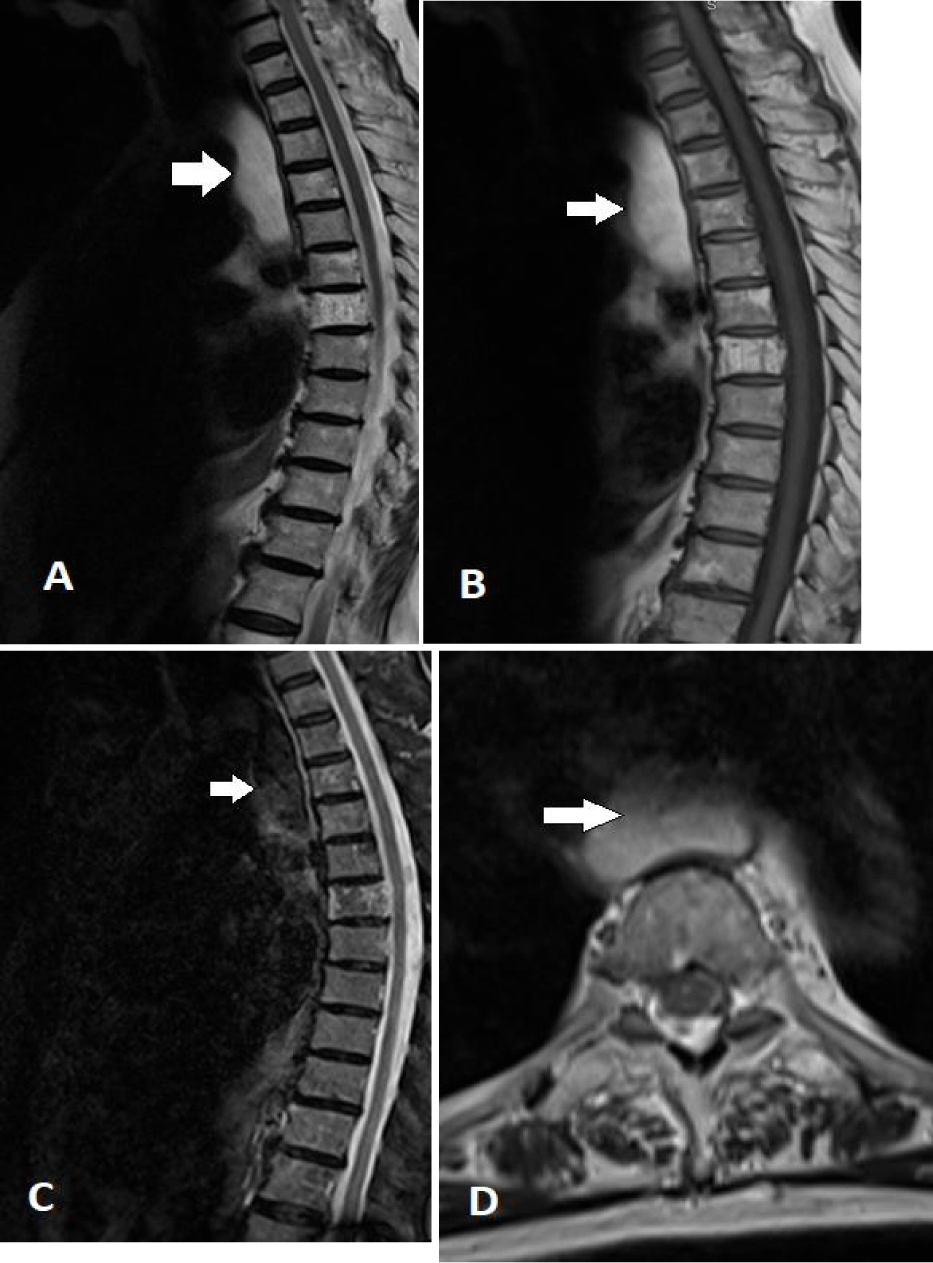
The mass was partially seen in an older MRI of the thoracic spine done 12 months prior to the CT scan, but not reported/documented (Figure 3). The family clinic then referred the patient to the GI clinic for further evaluation and upper GI endoscopy.
Discussion
Benign oesophageal tumours are rare, comprising less than 1% of all oesophageal neoplasms, which include leiomyomas, fibrovascular polyps, squamous papilloma, granular cell tumours, lipomas, neurofibromas, and inflammatory fibroid polyps. Lipomas in the alimentary tract comprise 4.1% of all benign tumours, and oesophageal lipomas represent only 0.4% of all benign GI tract neoplasms [1,2].
Lipomas can occur throughout the GI tract, most frequently in the colon and small intestine and less commonly in the oesophagus and stomach [3]. Oesophageal lipomas typically arise from the oesophagus' cervical and upper thoracic regions [4]. They are most seen in individuals in their 50s to 70s, with a slight predominance in females [5]. These benign tumours are generally asymptomatic and often found incidentally (~85%) [4]. The size of a lipoma influences its potential to cause symptoms. According to Hurwitz MM, et al. [6] GI tract lipomas under 1 cm are usually asymptomatic, whereas 75% of those over 4 cm may cause symptoms. Lipomas exceeding 2 cm in diameter can produce symptoms such as dysphagia, regurgitation, recurrent melena, and epigastric pain [6,7]. The most common symptom is dysphagia. However, 85% of oesophageal lipomas are clinically silent, with most cases discovered incidentally through radiographic imaging [5].
Accurate diagnosis requires a comprehensive examination, imaging techniques (such as barium swallow, CT chest, and MRI), and upper GI endoscopy [8]. On a CT scan, lipomas appear as homogeneous fat-density lesions (-40 to -120 HU) [9]. MRI reveals lipomas as T1-weighted hyperintense areas that become hypointense on fat-suppressed images [10]. Conversely, liposarcomas are heterogeneous with high signal intensity on T1 and T2-weighted images [11]. Taylor AJ, et al. [5] noted that strands within a homogeneous fatty tumour may be due to inflammatory changes and should not be mistaken for liposarcoma, a rare occurrence.
The management of oesophageal lipoma depends on symptoms, tumour location, and available expertise. General anesthesia is typically used for surgeries, including necessary endoscopic procedures. For smaller tumours, flexible or rigid upper endoscopy is effective, often guided by Endoscopic Ultrasound (EUS) to confirm mass location, allowing for procedures like polypectomy or endomucosal resection [12]. Most cases involve oesophagotomy and excision, while large tumours or those at the gastroesophageal junction may necessitate oesophagectomy. Surgical approaches include open surgery or Minimally Invasive Techniques (MIS). A left cervical open approach is used for cervical lesions [13], while Video-Assisted Thoracoscopic Surgery (VATS), Robotic-Assisted Thoracoscopic Surgery (RATS), and laparoscopy are employed for mid, lower, and lower oesophageal masses, respectively [14,15]. The technique requires a longitudinal incision on the oesophagus, careful dissection to remove the tumour, and layered closure with a chest tube for monitoring postoperative complications. If complications are anticipated, conversion to thoracotomy may be recommended. Patients usually stay in the hospital for about three days, with potential complications including bleeding, oesophageal leaks, pneumothorax, surgical site infections, and tumour recurrence.
Conclusion
Oesophageal lipomas are infrequent and mostly asymptomatic, detected primarily through incidental imaging unless they grow large enough to cause obstructions like dysphagia. Diagnostic imaging through CT and MRI is crucial in identifying these benign tumours. Depending on the tumour's size and location, various treatment strategies can be considered, ranging from minimally invasive endoscopic approaches for upper oesophageal polyps to laparoscopic or thoracoscopic interventions for distal or intramural lesions, minimizing hospital stays and potential complications [11].
References
- MAYO CW, PAGTALUNAN RJ, BROWN DJ. Lipoma of the alimentary tract. Surgery. 1963 May;53:598-603. PMID: 13934160.
- Algin C, Hacioğlu A, Aydin T, Ihtiyar E. Esophagectomy in esophageal lipoma: report of a case. Turk J Gastroenterol. 2006 Jun;17(2):110-2. PMID: 16830292.
- Ferrari D, Bernardi D, Siboni S, Lazzari V, Asti E, Bonavina L. Esophageal Lipoma and Liposarcoma: A Systematic Review. World J Surg. 2021 Jan;45(1):225-234. doi: 10.1007/s00268-020-05789-4. Epub 2020 Oct 7. PMID: 33026474; PMCID: PMC7752877.
- Wang CY, Hsu HS, Wu YC, Huang MH, Hsu WH. Intramural lipoma of the esophagus. J Chin Med Assoc. 2005 May;68(5):240-3. doi: 10.1016/S1726-4901(09)70216-3. PMID: 15909732.
- Taylor AJ, Stewart ET, Dodds WJ. Gastrointestinal lipomas: a radiologic and pathologic review. AJR Am J Roentgenol. 1990 Dec;155(6):1205-10. doi: 10.2214/ajr.155.6.2122666. PMID: 2122666.
- Hurwitz MM, Redleaf PD, Williams HJ, Edwards JE. Lipomas of the gastrointestinal tract. An analysis of seventy-two tumors. Am J Roentgenol Radium Ther Nucl Med. 1967 Jan;99(1):84-9. PMID: 6016046.
- Tsalis K, Antoniou N, Kalfadis S, Dimoulas A, Dagdilelis AK, Lazaridis C. Laparoscopic enucleation of a giant submucosal esophageal lipoma. Case report and literature review. Am J Case Rep. 2013 May 31;14:179-183. doi: 10.12659/AJCR.883928. PMID: 23826462; PMCID: PMC3700497.
- Feldman J, Tejerina M, Hallowell M. Esophageal lipoma: a rare tumor. J Radiol Case Rep. 2012 Jul;6(7):17-22. doi: 10.3941/jrcr.v6i7.1015. Epub 2012 Jul 1. PMID: 23365708; PMCID: PMC3558046.
- Thompson WM. Imaging and findings of lipomas of the gastrointestinal tract. AJR Am J Roentgenol. 2005 Apr;184(4):1163-71. doi: 10.2214/ajr.184.4.01841163. PMID: 15788588.
- Borges A, Bikhazi H, Wensel JP. Giant fibrovascular polyp of the oropharynx. AJNR Am J Neuroradiol. 1999 Nov-Dec;20(10):1979-82. PMID: 10588130; PMCID: PMC7657802.
- Yang B, Shi PZ, Li X, Xu RJ. Well-differentiated liposarcoma of esophagus. Chin Med J (Engl). 2006 Mar 5;119(5):438-40. PMID: 16542592.
- Ferrari D, Aiolfi A, Bonitta G, Riva CG, Rausa E, Siboni S, Toti F, Bonavina L. Flexible versus rigid endoscopy in the management of esophageal foreign body impaction: systematic review and meta-analysis. World J Emerg Surg. 2018 Sep 12;13:42. doi: 10.1186/s13017-018-0203-4. PMID: 30214470; PMCID: PMC6134522.
- Maruyama K, Motoyama S, Okuyama M, Sasaki K, Sato Y, Hayashi K, Nanjo H, Ogawa J. Cervical approach for resection of a pedunculated giant atypical lipomatous tumor of the esophagus. Surg Today. 2007;37(2):173-5. doi: 10.1007/s00595-006-3357-8. Epub 2007 Jan 25. PMID: 17243042.
- Bernardi D, Ferrari D, Siboni S, Porta M, Bruni B, Bonavina L. Minimally invasive approach to esophageal lipoma. J Surg Case Rep. 2020 Jul 31;2020(7):rjaa123. doi: 10.1093/jscr/rjaa123. PMID: 32760482; PMCID: PMC7394138.
- Ferrari D, Bernardi D, Siboni S, Lazzari V, Asti E, Bonavina L. Esophageal Lipoma and Liposarcoma: A Systematic Review. World J Surg. 2021 Jan;45(1):225-234. doi: 10.1007/s00268-020-05789-4. Epub 2020 Oct 7. PMID: 33026474; PMCID: PMC7752877.
Content Alerts
SignUp to our
Content alerts.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.