Medicine Group. 2024 August 31;5(8):1063-1066. doi: 10.37871/jbres1989.
Spontaneous Breast Hematoma Induced by Vitamin K Antagonist Therapy: A Case Report
Amri M*, Altimimi A, Boudar A, Asklou A, Azzouzi L and Habbal R
- Spontaneous breast hematoma
- Vitamin K antagonists
- Anticoagulation
- Warfarin, Elderly patients
- Case report
Abstract
Anticoagulant medications, particularly Vitamin K Antagonists (VKAs), are essential for managing thrombotic conditions but can cause severe side effects such as spontaneous hematomas. This case report describes a 69-year-old woman on VKA therapy who developed a large right breast hematoma. Immediate suspension of VKA, blood transfusions, and vitamin K administration led to clinical improvement. Breast ultrasonography confirmed the diagnosis, and after a week, the hematoma regressed, allowing for the resumption of anticoagulation with unfractionated heparin. This case highlights the need for careful monitoring and management of VKA therapy, especially in elderly patients.
Introduction
Anticoagulant medications inhibit the spread of existing thrombi and prevent the development of new ones. These medications include standard (unfractionated) heparin, low molecular weight heparin, Direct-Acting Oral Anticoagulants (DOACs), fondaparinux, danaparoid, and Vitamin K Antagonists (VKAs). Anticoagulant treatment for mechanical prostheses is primarily based on VKAs, with warfarin sodium being the most widely used drug. Oral anticoagulants primarily block the final stage of producing factors VII, IX, and X, [1] inhibiting prothrombin, a vitamin K-dependent coagulation factor produced in the liver. However, these drugs can cause severe and unexpected side effects, including bleeding or hematoma in various anatomical regions [2]. The literature has only a few reports of Spontaneous Pectoral Hematomas (SPH) [3], a rare complication caused by VKA over-anticoagulation. We report a case of a spontaneous large right breast hematoma following VKA therapy for an aortic prosthesis in an elderly woman.
Patient and observation
A 69-year-old female patient with an aortic prosthesis for 3 years and on VKA therapy (Acenocoumarol 1 mg per day) presented to the emergency department with a 5-day history of gradually worsening right breast swelling and bruising. Clinical examination revealed that the patient was hemodynamically stable, with a blood pressure of 128/109 mmHg, a heart rate of 79 bpm, and normal oxygen saturation on room air. However, she exhibited anemia in her conjunctiva, indicating a possible reduction in hemoglobin levels. The patient had a BMI of 34 kg/m², classifying her as obese. Notably, she did not have any other known comorbidities or a history of chronic illness.
A month earlier, the patient had undergone a total hip replacement surgery for the right hip following a fall. This surgery had required postoperative pain management, and she was prescribed Anti-Inflammatory medications (NSAIDs). These medications may have potentiated the anticoagulant effects of the VKAs, increasing the risk of bleeding complications. The patient was not taking any other medications apart from the VKA (Acenocoumarol) and the NSAIDs.
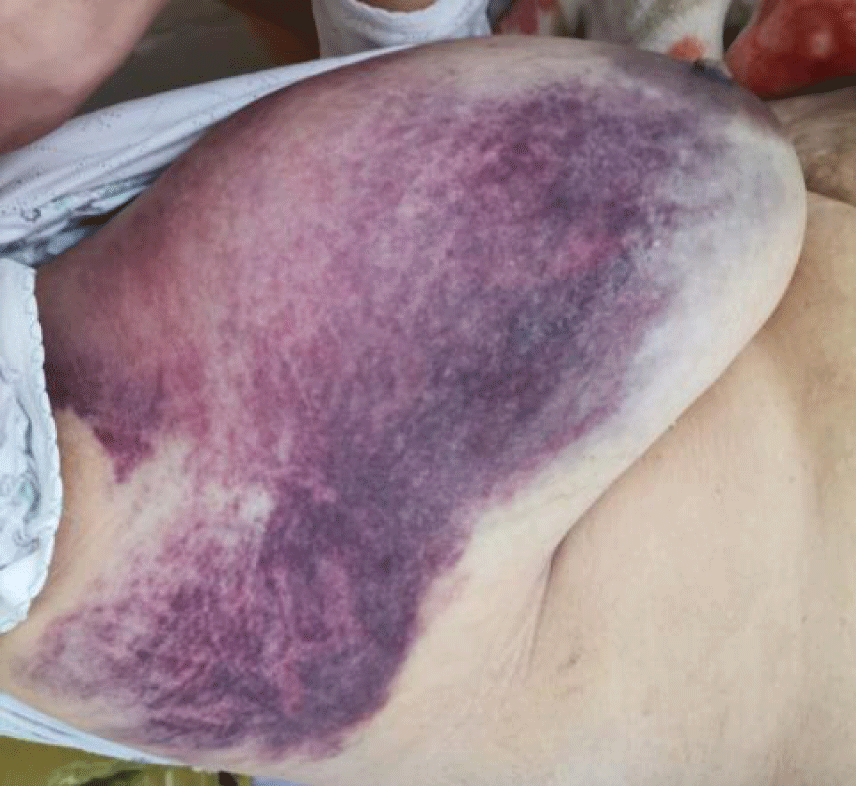
Clinically, there was a hematoma of the right breast extending to the axillary hollow and the dorsal side of the scapula, with a linear hematoma on the left breast (Figure 1).
Laboratory investigations revealed severe anemia (hemoglobin 6.1 g/dl), a markedly high international normalized ratio of prothrombin (INR > 8), and renal failure (creatinine 29.8 mg/l). The platelet count and liver function test were within normal ranges.
Immediate suspension of VKA was done, and the patient received three units of Red Blood Cells (RBC) and 10 mg of vitamin K. Breast ultrasonography confirmed the diagnosis by identifying a hematic collection measuring 13.4 × 7.16 cm, with no solid mass or malignancy detected. Transthoracic echocardiography revealed a functioning aortic prosthesis with an effective area of 1.8 cm², an aortic gradient of 17 mmHg, an acceleration time of 91 ms, and a patency index of 56%.
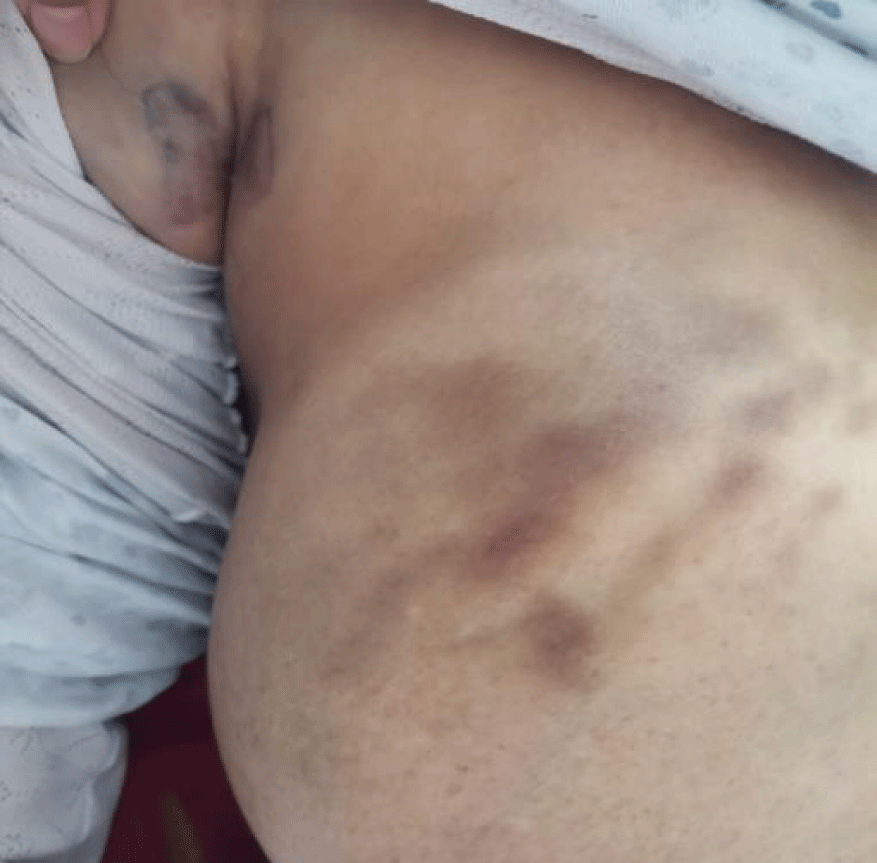
After a one-week therapeutic window, the hematoma regressed clinically (Figure 2) and echocardiographically. Biologically, control hemoglobin was 10.2 g/dL after a total transfusion of five red blood cells, and the INR was 1.85. We resumed Intra-Hospital Anticoagulant (UFH).
Discussion
Warfarin is the most widely used oral anticoagulant in Morocco due to its lower cost compared to DOACs and its suitability for patients with mechanical prostheses. Morocco has a high incidence of rheumatic diseases, and only VKAs like warfarin are approved for oral anticoagulation in these cases.
While effective, warfarin treatment carries a significant risk of hemostasis-related side effects. Hematomas are commonly seen in the skin, gastrointestinal system, abdomen, back, and legs, but they are rare in the breasts. Untreated breast hematomas can lead to skin necrosis and potentially necessitate a mastectomy. The clinical presentation varies depending on the hematoma's volume, ranging from small and asymptomatic to large and severe, potentially causing hemorrhagic shock [4].
Diagnostic methods include ultrasound, mammography, CT scan, MRI, and breast biopsy. CT and ultrasound are the most utilized techniques for a conclusive diagnosis. In our case, breast ultrasound was sufficient for diagnosis. Further imaging is required until the hematoma's full clinical and imaging resolution is documented. A biopsy is advised if a residual mass or mammographic anomaly persists after the hematoma resolves.
The treatment of SPH can be conservative or invasive, depending on the patient's condition. Supportive therapy is crucial, including ceasing anticoagulation, blood transfusions, and administering vitamin K, FFP, and prothrombin complex concentrate. Conservative care is preferred if the patient is hemodynamically stable. This approach was also followed in the case report by the Iranian team [5], where conservative treatment was chosen due to the patient's stability and the positive progress with the gradual regression of the hematoma. Invasive measures, such as open surgery or transcatheter arterial embolization, are necessary when conservative treatment fails or uncontrolled bleeding occurs. This approach is exemplified by the Turkish team [6], where the breast hematoma was extensive, leading to a preference for surgical intervention.
Preventing VKA-induced hematomas involves recognizing risk factors such as age [7], as demonstrated in the Iranian case report where the 80-year-old patient experienced increased vascular fragility.
Additional risk factors include comorbidities such as liver disease or renal failure, which further elevate the hemorrhagic risk. Drug interactions also play a significant role; VKAs used alongside medications like antiplatelets, NSAIDs, or certain antibiotics can increase bleeding risk. Indeed, antiplatelet drugs, such as aspirin or clopidogrel, inhibit platelet aggregation, which, when combined with VKAs, can lead to a higher risk of bleeding due to the combined effect on blood clotting [8]. NSAIDs, [9] on the other hand, not only affect platelet function but also can cause gastrointestinal mucosal damage, compounding the bleeding risk. Certain antibiotics [10] may alter the metabolism of VKAs by affecting liver enzymes or gut flora, which can lead to increased anticoagulant activity and a higher risk of bleeding complications. In the Moroccan case from Oujda [11], the interaction with Amoxicillin-Clavulanate and the patient’s renal failure exacerbated the effects of VKA therapy. In our case, the use of anti-inflammatory drugs was identified as a precipitating factor.
Switching to anticoagulants with a lower bleeding risk, such as DOACs, is an option when possible, although it was not available for our patient with a prosthetic valve. Other anticoagulants also carry risks, as documented in cases involving rivaroxaban and heparin.
Indeed, in 2017, Ming-Yang Li, et al. [12] research group from China documented a case involving a 71-year-old woman who developed a spontaneous hematoma while on rivaroxaban. The diagnosis was confirmed via ultrasound, and the treatment approach consisted of puncture drainage. Spontaneous breast haematoma was also described after heparin anticoagulation [13] and was successfully managed with cessation of anticoagulation, protamine, desmopressin and blood transfusion.
Conclusion
Spontaneous pectoral hematoma is a rare complication of VKA over-anticoagulation, underscoring the need for careful monitoring and cautious prescribing, especially in elderly patients with multiple conditions. DOACs are generally preferable for patients with challenging INR management, offering at least equivalent efficacy to warfarin with a lower bleeding risk. Close observation is usually sufficient for severe breast hematomas, and invasive treatments should be avoided unless necessary. Effective use of newer anticoagulants can help reduce complications. If a hematoma persists with abnormal findings, a biopsy is recommended to rule out malignancy.
No Conflict of Interest
Patient consent was obtained prior to the publication of this article.
References
- Kayaalp SO. Medical pharmacology for rational treatment. Ankara: Pelikan Publishing. 2012.
- Yang JC, Makaryus AN. Warfarin Anticoagulation and Spontaneous Pectoral Haematomas. Heart Lung Circ. 2016 Jul;25(7):e81-4. doi: 10.1016/j.hlc.2015.10.022. Epub 2016 Feb 8. PMID: 26948766.
- Gani I, Kapoor R, Saeed M. Spontaneous Breast Haematoma after Heparin Anticoagulation. Eur J Case Rep Intern Med. 2020 Jun 11;7(9):001735. doi: 10.12890/2020_001735. PMID: 32908833; PMCID: PMC7473684.
- Patel N, Baker SM, Modrykamien A. Hemorrhagic shock due to spontaneous pectoral hematoma associated with anticoagulation therapy. J Gen Intern Med. 2013 Dec;28(12):1673. doi: 10.1007/s11606-013-2451-z. Epub 2013 May 1. PMID: 23636915; PMCID: PMC3832720.
- Shakerian B, Razavi N. Warfarin-Induced Spontaneous Bilateral Breast and Extrathoracic Hematoma in an Elderly Woman. J Tehran Heart Cent. 2020 Apr;15(2):84-85. doi: 10.18502/jthc.v15i2.4190. PMID: 33552201; PMCID: PMC7825465.
- Gündeş E, Değer KC, Taşcı E, Senger AS, Duman M. Anticoagulant-induced breast hematoma. Ulus Travma Acil Cerrahi Derg. 2017 Jan;23(1):72-73. doi: 10.5505/tjtes.2016.01657. PMID: 28261775.
- Beyth RJ, Landefeld CS. Anticoagulants in older patients. A safety perspective. Drugs Aging. 1995 Jan;6(1):45-54. doi: 10.2165/00002512-199506010-00004. Erratum in: Drugs Aging 1995 Apr;6(4):343. PMID: 7696778.
- Patel MR. The role of antiplatelet therapy in the management of cardiovascular disease. American Journal of Cardiology. 2011;108(1):24-33.
- Lanas A. NSAID-induced gastrointestinal damage and the role of proton pump inhibitors. Nature Reviews Gastroenterology & Hepatology. 2011;8(8):481-493.
- Maree AO. The effect of antibiotic therapy on the INR in patients on stable warfarin therapy. Journal of Clinical Pharmacy and Therapeutics. 2010;35(5):499-504.
- Benbouchta K, Mrabet A, Kallel O, El Ouafi N, Bazid Z. Spontaneous massive pectoral hematoma induced by vitamin K antagonist therapy: a case report. Pan Afr Med J. 2021 Apr 1;38:324. doi: 10.11604/pamj.2021.38.324.28454. PMID: 34285747; PMCID: PMC8265252.
- Ming-Yang Li, Xiao-Ping Li, Hai-Xian Ren, Shi-Hui Tang, Booreddy S, Can-Can Zhang, Zhi-Jun Tan. Rivaroxaban-induced breast spontaneous hematoma: A case report. Int J Clin Exp Med. 2018;11(6):6378-6382.
- Gani I, Kapoor R, Saeed M. Spontaneous Breast Haematoma after Heparin Anticoagulation. Eur J Case Rep Intern Med. 2020 Jun 11;7(9):001735. doi: 10.12890/2020_001735. PMID: 32908833; PMCID: PMC7473684.
Content Alerts
SignUp to our
Content alerts.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.