Medicine Group. 2024 August 21;5(8):1009-1011. doi: 10.37871/jbres1982.
Biliary Colic. Is it All?
Sapunov VB*
- Abdominal pain
- Icterice
- Ultrasound
Abstract
We present a very common case about abdominal pain, but with some peculiarity that we consider notable. The use of ultrasound in Primary Care consultation was very useful to reach the final diagnosis among the multiple possible differential diagnoses.
Introduction
Abdominal pain is a very frequent reason Primary Care consultation in. Its multiple causes range from a vital emergency, which requires immediate surgical treatment, to self-limiting conditions that require only analgesic treatment [1,2]. 20% of cases end up being diagnosed as “nonspecific abdominal pain.” Therefore, making a correct differential diagnosis is very complicated. Even more so if we add the difficulty for patients to define the pain characteristics they present.
Pain in the right upper quadrant is generally related to a hepatobiliary origin: biliary colic, cholecystitis or cholangitis. Clinically they are characterized by the sudden appearance of epigastric pain and/or pain in the right upper quadrant, with or without nausea and vomiting. Its cause is usually a lithiasis that obstructs the cystic or common bile duct.
We present a very common case, but with some peculiarity that we consider notable: 47-year-old woman who consults by telephone due to dyspepsia of 2 months' duration; A week ago she began to have intermittent epigastric pain, vomiting after eating and feeling dysthermic. If there is a first suspicion of gastroenteritis, we recommend that she attend the consultation in person.
She presents marked icterice of the skin and mucous membranes, and reports no pain at the time of the examination, which is completely normal. Expanding the history, the patient reported generalized pruritus and coluria for several days.
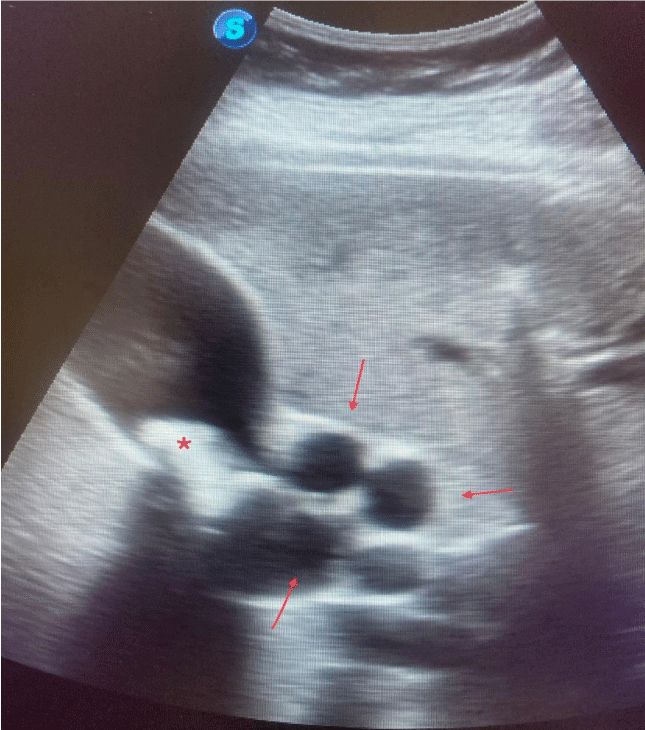
Thinking about a possible cholestatic syndrome, we performed an abdominal ultrasound in the same consultation. Where we clearly appreciate the presence of a lithiasis lodged in the infundibulum of the gallbladder along with dilation and tortuosity of the common bile duct (Figure 1).
Despite not reporting pain, due to the jaundice he had and the results of the ultrasound, we referred him to the hospital emergency department for evaluation and study.
The patient was admitted to the Digestive Service, where she underwentan Endoscopic Retrograde Cholangiopancreatography (ERCP) with placement of a common bile duct stent, which freed the bile duct. And, later, a cholecystectomy was performed. She was discharged with the diagnosis of Mirizzi Syndrome, remaining completely asymptomatic.
Mirizzi Syndrome (MS) is a rare complication of cholelithiasis (present in 0.1% of patients with gallbladder disease and in 0.7-2.7% of cholecystectomies performed) [2-5].It is characterized by a condition of obstructive jaundice secondary to the impaction of cholelithiasis in the infundibulum of the gallbladder or the cystic duct, which externally compresses the common hepatic duct, potentially causing a cholecystole fistula.coledociana [6]. It is associated with a higher incidence of gallbladder cancer compared to those patients who present isolated cholelithiasis, possibly because it causes chronic inflammation of the bladder wall [3,7,8].
Its diagnosis is very difficult, since it lacks pathognomonic signs and symptoms. As differential diagnoses we must include all causes of obstructive jaundice. It is common for patients to report long-standing biliary symptoms, presenting clinical and biochemical signs of biliary obstruction at the time of diagnosis. Pain in the right upper quadrant, although common, is not always present (Murphy's sign can be positive in 50% of cases) and almost 60% can present with an acute infectious condition: cholecystitis, cholangitis or pancreatitis [4].
The initial screening method is abdominal ultrasound, which has a sensitivity of up to 27% and a specificity of 90% and, if the diagnosis is suspected, it is confirmed by ERCP, whose sensitivity is 76 to 100% 8. This test, while diagnostic, is a therapeutic technique [3].
Ultrasound signs that would indicate the possibility of MS are: contracted gallbladder with dilated intrahepatic bile duct and common hepatic duct. The caliber of the common bile duct being normal. MS is also suggested by dilation of the neck of the gallbladder, the presence of impacted cholelithiasis at the level of the neck of the gallbladder, or the abrupt change in the width of the common hepatic duct distal to cholelithiasis [9].
The definitive treatment is cholecystectomy [3,4,8]. Placing a common bile duct stent using ERCP is a bridging method to surgery in cases of significant hyperbilirubinemia, as occurred in the case at hand [8].
Conclusion
In summary, MS is a rare complication of biliary pathology (0.1%). This low incidence and the fact that the published series consist of very few patients justifies the difficulty of its diagnosis. In Primary Care, it is usually a chance finding. However, its frequent association with gallbladder cancer forces its diagnosis to be considered in the presence of obstructive jaundice with the peculiarities previously mentioned; Therefore, it is necessary to suspect it, being attentive to the signs and symptoms described and having the necessary equipment to be able to perform and interpret an ultrasound on an outpatient basis.
References
- Ugarte MJ. Enfrentamiento del paciente con dolor abdominal. Revista Médica Clínica Las Condes. 2021;32(4):457-465.
- Palacios D, Gutierrez My, Gordillo FJ. Síndrome de Mirizzi, una causa infrecuente de ictericia obstructiva. Semergen. 2011;37(3):167-169. doi: 10.1016/j.semerg.2010.10.008.
- Jones MW, Ferguson T. Mirizzi syndrome. In: StatPearls, editor. Treasure Island (FL): StatPearls Publishing; 2024.
- Klekowski J, Piekarska A, Góral M, Kozula M and Chabowski M. The Current Approach to the Diagnosis and Classification of Mirizzi Syndrome. Diagnostics (Basel). 2021 Sep 10;11(9):1660. doi: 10.3390/diagnostics11091660. PMID: 34574001; PMCID: PMC8465817.
- Pemberton M, Wells AD. The Mirizzi syndrome. Postgrad Med J. 1997 Aug;73(862):487-90. doi: 10.1136/pgmj.73.862.487. PMID: 9307740; PMCID: PMC2431374.
- Safioleas M, Stamatakos M, Safioleas P, Smyrnis A, Revenas C and Safioleas C. Mirizzi Syndrome: an unexpected problem of cholelithiasis. Our experience with 27 cases. Int Semin Surg Oncol. 2008 May 21;5:12. doi: 10.1186/1477-7800-5-12. PMID: 18495037; PMCID: PMC2413250.
- Ramia JM, Villar J, Muffak K, Mansilla A, Garrote D, Ferron JA. Síndrome de Mirizzi y cáncer de vesícula [Mirizzi syndrome and gallbladder cancer]. Cir Esp. 2007 Feb;81(2):105-6. Spanish. doi: 10.1016/s0009-739x(07)71274-5. PMID: 17306129.
- Alemi F, Seiser N, Ayloo S. Gallstone Disease: Cholecystitis, Mirizzi Syndrome, Bouveret Syndrome, Gallstone Ileus. Surg Clin North Am. 2019 Apr;99(2):231-244. doi: 10.1016/j.suc.2018.12.006. PMID: 30846032.
- Turner MA, Fulcher AS. The cystic duct: normal anatomy and disease processes. Radiographics. 2001 Jan-Feb;21(1):3-22; questionnaire 288-94. doi: 10.1148/radiographics.21.1.g01ja093. PMID: 11158640.
Content Alerts
SignUp to our
Content alerts.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.