Medicine Group. 2024 August 12;5(8):980-982. doi: 10.37871/jbres1977.
Crystal-Induced Colitis Mimicking Crohn's Disease
Davi Viana Ramos1, Eloy Vianey Carvalho de França1, David Ramos da Silva2 and1*
2Department of Pathological Anatomy of Hospital of Clinics of Sao Paulo, Brazil
- Colitis
- Sevelamer
- Crohn's disease
- Chronic kidney disease
Abstract
Crystal-induced colitis, a rare complication of sevelamer therapy in Chronic Kidney Disease (CKD) patients, presents diagnostic challenges. We report a case of a 39-year-old man with severe lower gastrointestinal bleeding attributed to sevelamer-induced colonic ulcers. Despite initial suspicion of Crohn's disease, histopathological analysis revealed crystalline material suggestive of sevelamer-associated colitis. Discontinuation of sevelamer led to the cessation of bleeding and stabilization of the patient's condition. This case highlights the importance of considering medication-induced gastrointestinal complications in CKD patients.
Introduction
Chronic kidney disease, particularly in its terminal stage, leads to elevated phosphate levels, necessitating management with phosphate-binding medications such as sevelamer. Sevelamer, a non-calcium compound, reduces phosphate absorption in the gastrointestinal tract and promotes fecal excretion. Its unique calcium-free formulation differentiates it from other agents [1]. Common adverse effects include gastrointestinal symptoms since abdominal pain to severe complications like perforation and significant bleeding [2]. This paper discusses an unusual differential diagnosis of Crohn's disease in a case of lower gastrointestinal hemorrhage linked to sevelamer-induced colonic ulcers.
Case Report
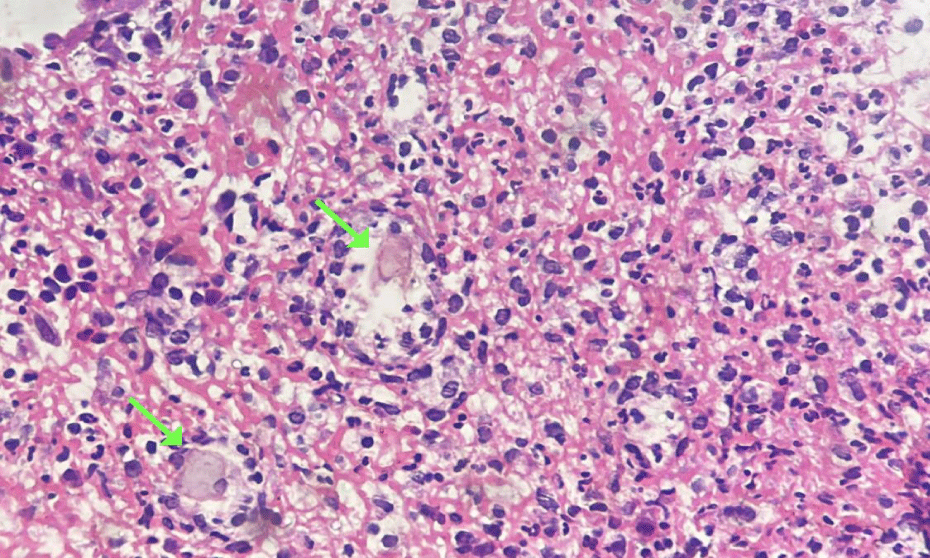
A 39-year-old man, post kidney transplant for focal segmental glomerulosclerosis, and on daily hemodialysis, presented to the emergency department with syncope and significant hematochezia, with hypotension and a drop in 3g/dL of hemoglobin levels. He was under treatment with sevelamer hydrochloride, calcium carbonate, acetylsalicylic acid, clopidogrel and vitamin D. Haemorrhagic shock was treated with blood transfusions and norepinephrine. Diagnostic tests showed no infectious pathogens, and EGD revealed mild gastritis. Despite the interruption of vasoactive drugs and blood transfusions, persistent hematochezia led to a colonoscopy, which revealed a cecum with multiple ulcers and friability (Figure 1), leading to suspicion of Crohn's disease. A histopathological analysis showed crystalline material under microscopy, suggestive of colitis associated with sevelamer (Figure 2). Discontinuation of sevelamer resulted in the cessation of bleeding and stabilization of his condition.
Discussion
Gastrointestinal lesions from medications are common but challenging to diagnose. Nonsteroidal anti-inflammatory drugs are well known for such effects, but medications such as sevelamer, which forms crystals, are increasingly recognized [2,3]. Sevelamer, an ion exchange resin for hyperphosphatemia, is generally safe but can cause serious gastrointestinal complications, with severe inflammation, formation of ulcers similar to those found in Crohn's disease and major bleeding [4-6]. Initial theories suggested ischemic events and colonic perforations were linked to mesenteric vasospasm, particularly under conditions like hypovolemia common in hemodialysis patients [7-10]. Later findings of sevelamer-like crystals in gastrointestinal lesions corroborate the direct damage potential of the medication.
Conclusion
Sevelamer-induced colitis is a rare but serious complication necessitating intensive care and can be life-threatening. With the increasing survival of renal transplant and renal replacement therapy patients, many are on long-term sevelamer therapy. Awareness of its potential complications and possible differential diagnoses, such as Crohn's disease, are crucial for timely intervention, potentially saving lives and avoiding emergency surgeries.
References
- Barna MM, Kapoian T, O'Mara NB. Sevelamer carbonate. Ann Pharmacother. 2010 Jan;44(1):127-34. doi: 10.1345/aph.1M291. Epub 2009 Dec 2. PMID: 19955298.
- Desai M, Reiprich A, Khov N, Yang Z, Mathew A, Levenick J. Crystal-Associated Colitis with Ulceration Leading to Hematochezia and Abdominal Pain. Case Rep Gastroenterol. 2016 Jun 27;10(2):332-7. doi: 10.1159/000446575. PMID: 27482192; PMCID: PMC4945809.
- Madan P, Bhayana S, Chandra P, Hughes JI. Lower gastrointestinal bleeding: association with Sevelamer use. World J Gastroenterol. 2008 Apr 28;14(16):2615-6. doi: 10.3748/wjg.14.2615. PMID: 18442219; PMCID: PMC2708383.
- Swanson BJ, Limketkai BN, Liu TC, Montgomery E, Nazari K, Park JY, Santangelo WC, Torbenson MS, Voltaggio L, Yearsley MM, Arnold CA. Sevelamer crystals in the gastrointestinal tract (GIT): a new entity associated with mucosal injury. Am J Surg Pathol. 2013 Nov;37(11):1686-93. doi: 10.1097/PAS.0b013e3182999d8d. PMID: 24061514.
- Lee ZJ, Chia C, Busmani I, Wong WK. A rare cause of ischemic gut: A case report. Int J Surg Case Rep. 2016;20:114-7. doi: 10.1016/j.ijscr.2016.01.018. Epub 2016 Jan 22. PMID: 26852360; PMCID: PMC4818320.
- Chintamaneni P, Das R, Kuan SF, Kermanshahi TR, Hashash JG. Hematochezia Associated with Sevalamer-Induced Mucosal Injury. ACG Case Rep J. 2014 Apr 4;1(3):145-7. doi: 10.14309/crj.2014.32. PMID: 26157856; PMCID: PMC4435309.
- Yamaguchi T, Ohyama S, Furukawa H, Sato N, Ohnishi I, Kasashima S, Kawashima A, Kayahara M. Sigmoid colon diverticula perforation associated with sevelamer hydrochloride administration: A case report. Ann Med Surg (Lond). 2016 Aug 2;10:57-60. doi: 10.1016/j.amsu.2016.07.020. PMID: 27547398; PMCID: PMC4983137.
- Keri KC, Veitla V, Samji NS. Ischemic Colitis in Association with Sevelamer Crystals. Indian J Nephrol. 2019 May-Jun;29(3):191-193. doi: 10.4103/ijn.IJN_80_18. PMID: 31142966; PMCID: PMC6521773.
- Fistrek Prlic M, Jelakovic M, Brinar M, Grgic D, Romic I, Marusic Z, Ivandic E, Jelakovic B, Vukovic Brinar I, Krznaric Z. Case report: Sevelamer-associated colitis-a cause of pseudotumor formation with colon perforation and life-threatening bleeding. Front Med (Lausanne). 2023 Apr 27;10:1097469. doi: 10.3389/fmed.2023.1097469. PMID: 37181355; PMCID: PMC10174228.
- Nambiar S, Pillai UK, Devasahayam J, Oliver T, Karippot A. Colonic Mucosal Ulceration and Gastrointestinal Bleeding Associated with Sevelamer Crystal Deposition in a Patient with End Stage Renal Disease. Case Rep Nephrol. 2018 Feb 28;2018:4708068. doi: 10.1155/2018/4708068. PMID: 29682371; PMCID: PMC5851163.
Content Alerts
SignUp to our
Content alerts.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.