Medicine Group . 2022 April 21;3(4):367-372. doi: 10.37871/jbres1450.
COVID-19 Community Survey, Knowledge, Attitude and Practice by Bangladeshi Population
Subrina Jesmin1,2*, Adil Maqbool3,4, Farzana Sohael5, Majedul Islam Md2,6, Yujiro Matsuishi2, Takeru Shima7, Nobutake Shimojo6, Satoru Kawano8, Arifur Rahman Md9, Naoto Yamaguchi8 and Masao Moroi1
2Health & Disease Research Centre for Rural Peoples (HDRCRP), Mohammadpur, Dhaka-1207, Bangladesh
3Allama Iqbal Medical College, University of Health Sciences (UHS) Lahore, Pakistan
4Jinnah Hospital, Lahore, Pakistan
5Department of Gynecology, Dhaka Medical College, Dhaka, Bangladesh
6Department of Emergency and Critical Care Medicine, Faculty of Medicine, University of Tsukuba, Tsukuba, Ibaraki,Japan.
7Department of Health and Physical Education, Cooperative Faculty of Education, Gunma University, Gunma, Japan
8Ibaraki Prefectural University of Health Sciences, Ami, Japan
9Shaheed Ziaur Rahman Medical College, Bogura, Bangladesh
- COVID-19 Bangladesh
- Knowledge
- Attitude
Abstract
Background: In a public health crisis, knowledge and understanding of disease transmission modes, fundamental hygiene concepts, and procedures are critical for designing effective control measures. The purpose of this research was to assess the Bangladeshi population's Knowledge, Attitude and Practice (KAP) towards COVID-19.
Methods: A series of questions about the KAP of the population about COVID-19 were asked in this cross-sectional study, which was conducted among the general population of Bangladesh over the age of 15, and participants' demographic characteristics and source of information about COVID-19 were recorded and analyzed.
Results: Despite the fact that the majority of respondents (more than 60%) had a positive attitude about COVID-19, 70% of those questioned in Bangladesh had insufficient understanding and preventative actions. This latter discovery is promising and suggests a potential therapeutic strategy. Male and less educated respondents reported inadequate COVID-19 preventive methods, as well as a lack of understanding about signs and symptoms and transmission. The findings revealed a substantial link between knowledge, attitude, and practice among women of a certain gender, age, and education level. Male gender, non-healthcare-related jobs, single status, and a lesser degree of schooling were all substantially correlated with poorer knowledge scores, according to multiple linear regression analysis.
Conclusion: The present study revealed a high attitude among the study population towards COVID-19 but a poor response on knowledge and preventive practices, which can be enhanced by awareness campaigns and proper planning.
Introduction
Coronavirus Disease (COVID-19), caused by the Severe Acute Respiratory Syndrome Coronavirus 2 (SARS-CoV-2) virus, is a worldwide pandemic that began in Wuhan, China, and soon spread to over 180 nations. As the new coronavirus evolves, our understanding of whom this virus will affect severely remains limited [1]. COVID-19 is presently one of the most serious worldwide health issues. The pandemic's spread has impacted numerous nations, producing issues in practically every facet of daily life. It has caused global economic realignment, exacerbated medical crises in many already fragile nations, and is presently the most widely covered issue in the media. For all healthcare systems across the globe, the pandemic offers an unprecedented challenge. This is the first medical disaster in modern history to strike several populations, regions, and continents, necessitating everyone's awareness and readiness [2]. SARC-CoV-2 was discovered in lower respiratory tract samples from afflicted individuals, according to a Chinese investigation. In February 2020, the newly identified virus was given the name COVID-19 [3]. This illness has become a huge public health issue across the world, causing widespread anxiety among people as it spreads swiftly over the globe [4]. The virus is very infectious and may quickly spread from person to person by respiratory droplets when infected persons sneeze or cough, and it can survive for many hours on the surface of various surfaces [5]. Contacting droplet-contaminated surfaces or items and then touching the eyes, nose, or mouth might readily transfer the virus to a healthy individual [6]. Fever, cough, malaise, and trouble breathing are the main clinical signs of COVID-19 [7]. While some have dubbed COVID-19 "the great equalizer," early reports from hard-hit regions in the United States indicate that the illness has a disproportionate impact on long-standing social determinants of health, such as racial/ethnic and socioeconomic inequality [8-10]. One of the first states to publish COVID-19 data by race/ethnicity and demographic factors was Michigan. Diabetes, hypertension, cancer, renal, lung, and heart disorders all increase the severity of the condition in elderly people [11]. In South Asia, especially Bangladesh, COVID-19 has shown significant gaps in public health preparation and response to infectious disease risks and outbreaks. [12] The absence of a robust public health monitoring system is especially noticeable. With over 160 million people, Bangladesh is one of the poorest and most densely inhabited nations on the planet [13]. The Institute of Epidemiology Disease Control and Research (IEDCR) detected the first COVID-19 case in Bangladesh on March 7, 2020 [14]. On March 9, 2020, the number of infected patients continued to climb, and by December 16, 2020, Bangladesh had recorded 494,209 infected cases and 7129 fatalities [14]. We are presently witnessing a global emergency impacting all cultures, and it has put billions of people under lockdown due to a lack of adequate treatment and vaccination for COVID-19. Desperate attempts are being made throughout the globe to stop the epidemic, which has resulted in the collapse of health systems and long-term geopolitical and economic consequences. Because there is currently no recognized medical therapy for the virus, social distance is the only viable option for halting its spread apart for the several vaccines, now available for COVID-19 [15]. Future outbreaks of CoVs are anticipated to be inevitable due to changes in climate and ecology, as well as greater human-animal contact. As a result, effective treatments and vaccines against CoVs are required [16]. According to retrospective research of middle-aged and older COVID-19 patients, the elderly are more sensitive to the disease and are more likely to be admitted to the ICU, with a greater fatality rate [17]. Alterations in lung structure and muscle atrophy may contribute to age-related changes in the elderly population, resulting in changes in physiologic function, a loss in lung reserve, a reduction in airway clearance, and a reduction in defensive barrier function [17].
Methods
The study included a total of 503 respondents from rural and urban areas Bogura, Bangladesh. The first questionnaires were gathered in March (August 5, 2021–November 6, 2021), which were gathered in two waves: at the beginning of the pandemic and during Bangladesh's most severe COVID-19 lockdown. Demographic characteristics of the sample are presented in (Table 1). The demographics, knowledge, attitudes, and behaviors parts of the survey were separated into four categories. The first component collected information about the respondent's employment, age, and current home. The second section assessed basic knowledge on COVID-19, including symptoms, infection pathways, and preventative strategies. The final section assessed people's dread of a pandemic and which lockdown limitations were the hardest to bear. The fourth section focuses on COVID-19 information sources. The fourth topic (affected bodily systems) had a single response option, but the other questions (symptoms, transmission pathways, preventive, what to do when experiencing symptoms, everyday life challenges, worries, information sources) were multiple choice questions with numerous answers.
Ethics and informed consent
The study was approved by the review board of our institution's research committee prior to survey participant’s enrolment. Each participant was given access to all study materials as well as assurances of complete confidentiality. Only those who granted their consent were included in the study.
Statistical analysis
To compare all demographic and clinical aspects between the two groups (COVID-19 positive and COVID-19 negative), the paired student's t-test and the Mann-Whitney test for normal and skewed continuous variables, respectively, were employed (IBM SPSS Statistics, version 20). For all categorical comparisons between the two groups, we used the chi-square test (STATA, version 10). In Tables and figures 1-4, data is presented as Mean S.D. or percentage. A P-value of 0.05 was considered statistically significant for all parameters in this study.
Results
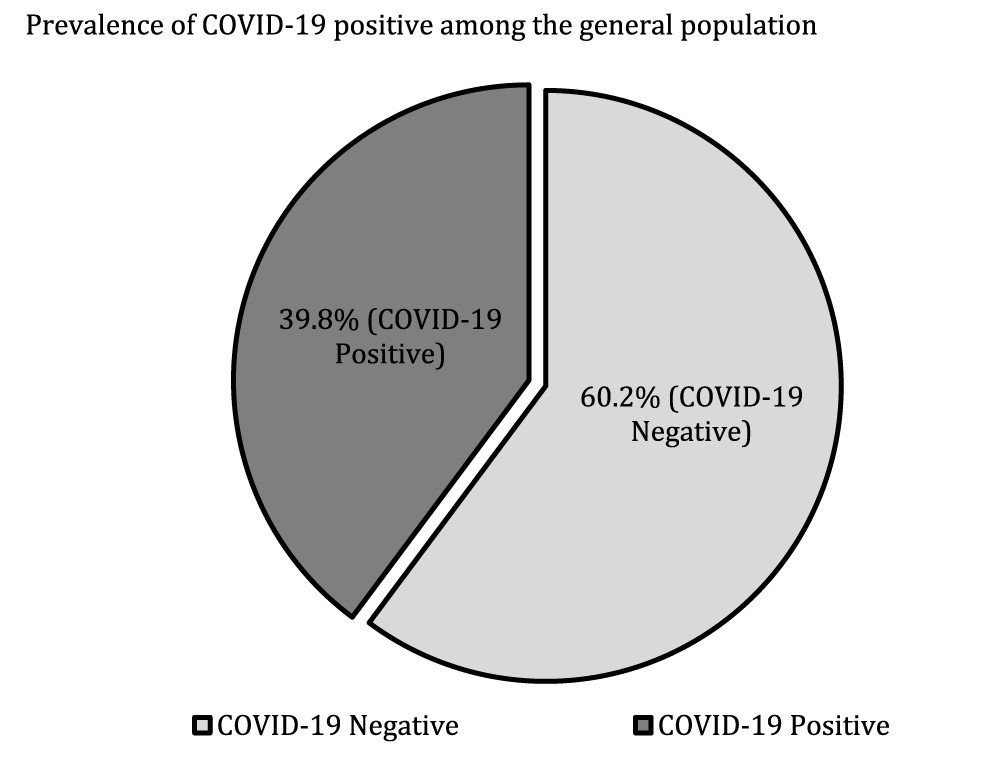
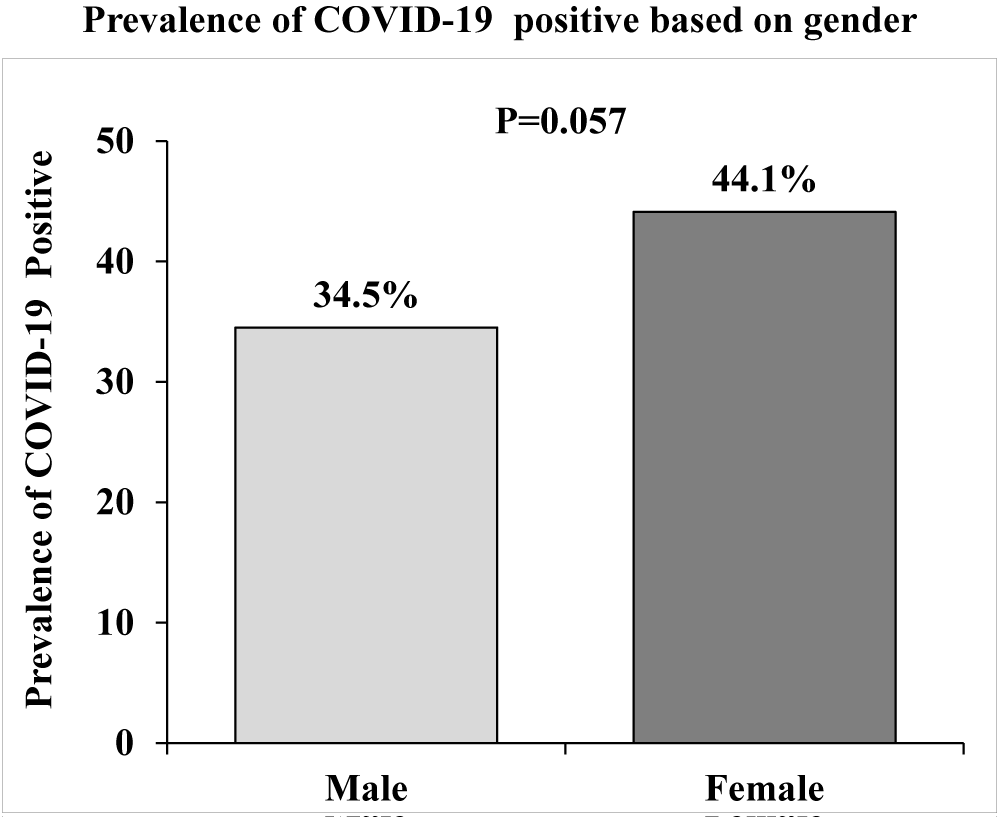
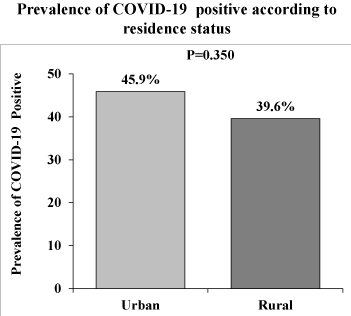
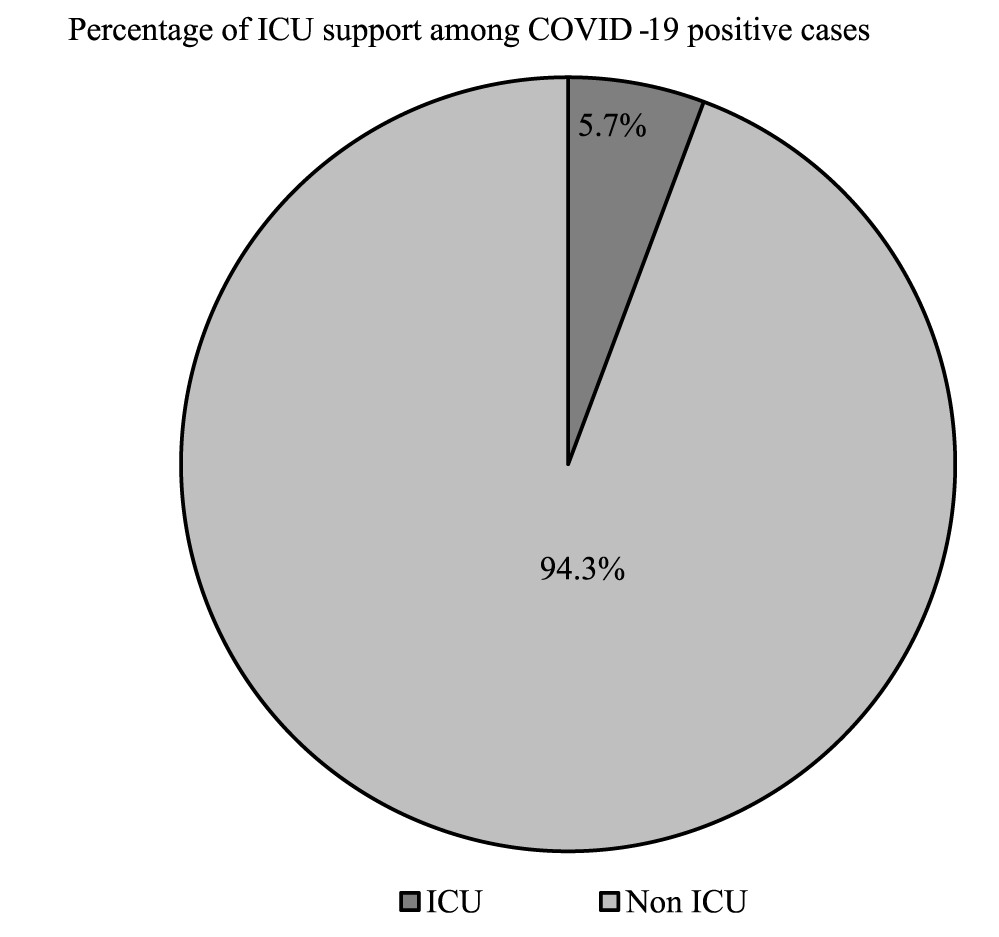
A total of 503 survey data were collected in Bangladesh both in rural and urban communities (Table 1). The mean age was 41.0 ± 14.7 years. The majority of the participants were Muslims by religion (94.9%), while the rest were Hindus (5.1%). A large number of the population was illiterate (41.6%). Most of the participants are married (89.3%). Among participants, 57.8% are housewives while others are self-employed (12.3%), doing government jobs (4.4%), and Business (25.0%). Most of them (24.2%) have tobacco consumption with a monthly income of less than 10,000 tk. (34.7%) while 65.3% have monthly income >= 10000 tk (Table 1). Out of these common symptoms, fever 67.3% showed up as the most common symptom, followed by dry cough in 52.9% patients. Other symptoms noted were Loss of taste or smell (16.0%), tiredness (30.0%), and difficulty breathing (65.6%). 42.4% of patients had diabetes mellitus, 27.0% had hypertension, and 13.2% of patients had ischemic heart disease, according to the Co-morbidity variable (Table 1). The prevalence of positive COVID-19 RT-PCR results is higher in females than in males (72.2% vs.27.8%, p = 0.057) (Table 2). There was a significant difference between positive and negative RT-PCR result for smoking habit (p = 0.005), weight (p = 0.001), height (p = 0.007), BMI (p < 0.001), ICU support (p = 0.018), O2 therapy (p = 0.025), fever (p < 0.001), dry cough (p < 0.001), headache (p < 0.001) and co-morbidity with COVID-19 patients. There was no significant difference in gender, residence status, waist circumference, body temperature, tiredness, loss of taste or smell, and ischemic heart disease in between positive or negative PCR result patients with COVID-19 (Table 2). Table 3 shows the association between the study subject's signs and symptoms and comorbidity characteristics and gender (male vs. female) of the COVID-19 general population, and the statistically significant result was in tiredness (p = 0.011) and headache (p = 0.041) by Chi-square analysis at p < 0.05. There was no significant difference between males and females for fever (p = 0.853), dry cough (p = 0.359), difficulty breathing (p = 0.684), loss of taste or smell (p = 0.709), and comorbidity with COVID-19 patients. Table 4 shows, age, gender, residence status, body temperature, Intensive Care Unit (ICU) support, O2 Therapy, diabetes mellitus and hypertension are statistically significant in binary logistic regression. The Odds Ratio (OR) for body temperature (F) was 0.97 (CI = 0.96-0.98, p < 0.001), for O2 Therapy was 1.75 (CI 1.35-2.26, p < 0.001), for hypertension was 1.32 (CI = 1.00-1.73, p < 0.047), for ischemic heart disease was 1.13 (CI 0.90-1.43, p < 0.291). Among relevant indicators, Intensive Care Unit (ICU) support (days) exhibited a higher odds ratio (OR 1.76, CI 1.37-2.27, p < 0.001) (Table 4).
| Table 1: Sociodemographic and clinical characteristics of study subjects (n = 503). | |
| Variable | Mean ± SD or number (%) |
| Age (years) | 41.0 ± 14.7 |
| Gender | |
| Male | 166 (33.8) |
| Female | 325 (66.2) |
| Anthropometric and behaviour parameters | |
| Weight (kg) | 64.6 ± 13.8 |
| Height (cm) | 152.5 ± 20.2 |
| Body mass index (kg/m2) | 29.3 ± 10.1 |
| Waist circumference (cm) | 102.8 ± 2.4 |
| Body temperature (F) | 99.3 ± 1.0 |
| Smoking habit (%) | 114 (31.3) |
| Tobacco consumption (%) | 86 (24.2) |
| Maternal educational level | |
| No education | 179 (41.6) |
| Primary education | 98 (22.8) |
| Secondary education | 116 (27.0) |
| Higher education | 37 (8.6) |
| Maternal marital status | |
| Unmarried | 39 (10.7) |
| Married | 327 (89.3) |
| Occupation | |
| Housewife | 21.9 (57.8) |
| Self-employment | 4.6 (12.3) |
| Government Job | 1.7 (4.4) |
| Business | 9.5 (25.0) |
| Others | 1 (0.5) |
| Monthly income (BDT) | |
| < 10000 | 34 (34.7) |
| > = 10000 | 64 (65.3) |
| Signs and symptoms | |
| Fever | 198 (67.3) |
| Dry cough | 108 (52.9) |
| Tiredness | 9 (30.0) |
| Difficulty breathing | 40 (65.6) |
| Loss of taste or smell | 8 (16.0) |
| Headache | 134 (54.9) |
| Co-morbidity | |
| Diabetes mellitus | 195 (42.4) |
| Hypertension | 91 (27.0) |
| Heart disease | 51 (13.2) |
| Liver disease | 34 (8.9) |
| Kidney disease | 37 (9.6) |
| Pulmonary disease | 49 (12.8) |
| Values are presented as mean ± SD for continuous variables and number (%) for categorical variables. Based on T-test for continuous variable and Pearson Chi-square test for categorical variable. SD: Standard Deviation |
|
| Table 2: Characteristics of respondents corresponding to COVID-19 status. | |||
| Variable | COVID-19 Positive | COVID-19 Negative | P value |
| Age (years) | 36.9 ± 12.3 | 44.2 ± 16.1 | < 0.001* |
| Gender | |||
| Male | 49 (27.8) | 93 (36.6) | 0.057 |
| Female | 127 (72.2) | 161 (63.4) | |
| Residence | |||
| Rural | 148 (84.1) | 226 (87.3) | 0.350 |
| Urban | 28 (15.9) | 33 (12.7) | |
| Smoking habit | 61 (37.0) | 31 (22.1) | 0.005* |
| Tobacco consumption | 46 (27.7) | 22 (16.7) | 0.024* |
| Weight (kg) | 66.5 ± 14.3 | 61.8 ± 12.9 | 0.001* |
| Height (cm) | 147.5 ± 21.6 | 153.3 ± 18.6 | 0.007* |
| Body mass index (kg/m2) | 32.5 ± 11.6 | 27.3 ± 8.7 | < 0.00* |
| Waist circumference (cm) | 102.7 ± 2.5 | 102.8 ± 2.5 | 0.956 |
| Body temperature (F) | 99.3 ± 1.2 | 99.2 ± 1.0 | 0. 872 |
| ICU support | 10 (5.7) | 0 (0.0) | 0.018* |
| O2 Therapy | 13 (7.5) | 1 (1.1) | 0.025* |
| Signs and symptoms | |||
| Fever | 117 (92.1) | 56 (39.4) | < 0.001* |
| Dry cough | 65 (90.3) | 38 (30.2) | < 0.001* |
| Tiredness | 6 (37.5) | 3 (21.4) | 0.338 |
| Difficulty breathing | 18 (66.7) | 1 (7.7) | < 0.001* |
| Loss of taste or smell | 5 (35.7) | 1 (14.3) | 0.306 |
| Headache | 78 (91.8) | 48 (38.4) | < 0.001* |
| Co-morbidity | |||
| Diabetes mellitus | 106 (65.8) | 56 (23.0) | < 0.001* |
| Hypertension | 49 (29.0) | 20 (18.0) | 0.037* |
| Ischemic heart disease | 20 (11.5) | 16 (10.5) | 0.781 |
| Liver disease | 17 (9.8) | 6 (4.0) | 0.042* |
| Kidney disease | 19 (10.9) | 5 (3.3) | 0.008* |
| Pulmonary Disease | 27 (15.7) | 9 (6.0) | 0.006* |
| Asthma | 10 (31.2) | 15 (15.5) | 0.050* |
| Chest pain | 122 (71.8) | 68 (29.1) | < 0.001* |
| Values are presented as mean ± SD for continuous variables and number (%) for categorical variables. Based on T-test for continuous variable and Pearson Chi-square test for categorical variable. COVID-19: Coronavirus Disease-2019; SD: Standard Deviation; *p < 0.05. |
|||
| Table 3: Differences of signs and symptoms and co-morbidity between male and female. | |||
| Variable | Male | Female | P value |
| Signs and symptoms | |||
| Fever | 64 (68.1) | 134 (67.0) | 0.853 |
| Dry cough | 38(57.6) | 70(50.7) | 0.359 |
| Tiredness | 8 (50.0) | 1 (7.1) | 0.011* |
| Difficulty breathing | 15(62.5) | 25(67.6) | 0.684 |
| Loss of taste or smell | 4(18.2) | 4(14.3) | 0.709 |
| Headache | 37 (45.7) | 97 (59.5) | 0.041* |
| Co-morbidity | |||
| Diabetes mellitus | 61 (40.4) | 134(43.4) | 0.545 |
| Hypertension | 34 (29.1) | 57 (25.9) | 0.535 |
| Ischemic heart disease | 23 (17.2) | 28 (11.2) | 0.101 |
| Liver disease | 11(8.3) | 23 (9.3) | 0.743 |
| Kidney disease | 8(6.0) | 29(11.6) | 0.073 |
| Pulmonary Disease | 17 (13.0) | 32 (12.9) | 0.972 |
| Asthma | 17 (26.2) | 23 (23.5) | 0.697 |
| Chest pain | 74 (47.7) | 151 (49.3) | 0.745 |
| Values are presented as number (%).Based on Pearson Chi-square test. *p < 0.05. | |||
| Table 4: Univariate regression analysis corresponding to COVID-19 (negative vs. positive). | |||
| Variable | Regression analysis | ||
| Odds ratio (OR) | 95% CI | P Value | |
| Age (years) | 0.99 | 0.98 - 0.99 | < 0.001* |
| Gender | 0.79 | 0.62 - 0.99 | 0.046* |
| Residence status | 0.65 | 0.53 - 0.81 | < 0.001* |
| Body temperature (F) | 0.97 | 0.96 - 0.98 | < 0.001* |
| Intensive care unit (ICU) support | 1.76 | 1.37 - 2.27 | < 0.001* |
| O2 Therapy | 1.75 | 1.35 - 2.26 | < 0.001* |
| Smoking habit | 0.95 | 0.73 - 1.25 | 0.732 |
| Tobacco consumption | 1.09 | 0.84 - 1.41 | 0.510 |
| Diabetes mellitus | 0.29 | 0.22 - 0.40 | < 0.001* |
| Hypertension | 1.32 | 1.00 - 1.73 | 0.047* |
| Ischemic heart disease | 1.13 | 0.90 - 1.43 | 0.291 |
| COVID-19: Coronavirus Disease-2019; CI: Confidence Interval; *p < 0.05. Based on binary logistic regression. | |||
Discussion
The intensity of the disease, the severity of its dissemination, and the mortality rate may all impact people's knowledge, attitudes, and practices when it comes to an infectious disease. Since the World Health Organization declared COVID-19 a pandemic, awareness, attitudes, and behaviors around COVID-19 have risen steadily. This research was carried out in Bangladesh and abroad during the start of the COVID-19 epidemic. Despite the fact that the majority of respondents (more than 60%) had a positive opinion about COVID-19, 70 percent of those polled in Bangladesh had insufficient awareness and preventative actions [18]. This latter discovery is promising and suggests a potential therapeutic strategy. Male and less educated respondents reported inadequate COVID-19 preventive methods, as well as a lack of understanding about signs and symptoms and transmission. In Bangladesh, moreover, half of the respondents said they had "excellent awareness" of COVID-19, with age and education having a major influence on knowledge and preventative activities [19]. COVID-19 is now a worldwide health hazard that has people worried [20]. Even though vaccination studies are underway, and several vaccines are available for COVID-19. But to battle this pandemic better we have to take more measures. Therefore, boosting community knowledge, attitude, and behaviors concerning COVID-19 is an important way to avoid the illness [21]. The goal of this research was to evaluate the communities' knowledge, attitudes, behaviors, and government restriction policy for preventing COVID-19 in Bangladesh. The COVID-19 pandemic is a fast expanding worldwide menace that affects everyone, regardless of occupation or age, in some manner. The COVID-19 pandemic is a fast expanding worldwide menace that affects everyone, regardless of occupation or age, in some manner. The research described in this article was a spontaneous and swift response to a unique and novel social situation, with the goal of gaining a better understanding of Bangladesh's population's awareness of and responses to the pandemic during two distinct stages of its growth. According to the findings, the government must make significant efforts to spread knowledge, attitudes, and practices about COVID-19 to the public, particularly regarding specific control measures such as wearing masks, the role of a few herbs in preventing infection, and the ineffectiveness of antibiotics in COVID-19 treatment. The latter is critical since it will undoubtedly aid in the battle against bacterial resistance, which is a serious public health issue worldwide, as well as offering appropriate herbal guidance. We think that the Ministry of Health and general practitioners should devote significant resources to teaching the public about COVID-19 via social media and television, which are the primary sources of information for more than half of the research participants. Increasing public awareness about the disease may aid in correcting some incorrect information people have about the disease, as seen in this study, where a few participants believed that smoking or taking antibiotics would prevent infection, and others thought COVID-19 infection and quarantine was a stigma and thus would hide their infection. They might be a source of infection, which would very certainly end in death.
Limitations
One of the limitations of this research was that the respondents might offer socially desired replies. Another limitation of this research was that we were unable to compare the respondents' knowledge, attitudes, and behaviors across age groups, gender, education, marital status, and profession. Another limitation of this research was the lack of uniformity of the measures we used to evaluate the respondents' knowledge, attitudes, and behaviors.
Conclusion
To conclude, the current research found that the study population had a positive view regarding COVID-19. Such a reaction shows the impact of the WHO's declaration of the COVID-19 as a pandemic, as well as efforts were undertaken by local health authorities to educate a broad range of the public about the virus. However, since a large majority of participants were illiterate, their responses to knowledge and prevention practices concerning COVID-19 were inadequate, necessitating the urgent need for media and mass communication-based awareness initiatives. The results of this research might serve as a foundation for developing public awareness campaigns and directing the efforts and strategies of the country's health authorities to control COVID-19 better and prevent its spread.
Acknowledgment
We would like to express our gratitude to every one of the interview participants who graciously provided us with the information we needed.
Financial Disclosure
This research has been partly supported by the grant from Ministry of Education and Science (2 1 K 0 7 3 5 4) in Japan.
Conflict of Interest
The authors declare that they have no conflict of interest.
Informed Consent
All study participants provided written informed consent.
Author Contributions
SJ has designed and executed the study. SJ has also drafted the manuscript. AM, FS, MMI, YM, NS, SK, MAR, NY and MM have assisted in sample collection and analysis. SJ and TS supervised this manuscript preparation and provided critical editing.
References
- Sanyaolu A, Okorie C, Marinkovic A, Patidar R, Younis K, Desai P, Hosein Z, Padda I, Mangat J, Altaf M. Comorbidity and its Impact on Patients with COVID-19. SN Compr Clin Med. 2020;2(8):1069-1076. doi: 10.1007/s42399-020-00363-4. Epub 2020 Jun 25. PMID: 32838147; PMCID: PMC7314621.
- Nazar W, Leszkowicz J, Pieńkowska A, Brzeziński M, Szlagatys-Sidorkiewicz A, Plata-Nazar K. Before-and-after online community survey on knowledge and perception of COVID-19 pandemic. BMC Infect Dis. 2020 Nov 19;20(1):861. doi: 10.1186/s12879-020-05602-6. PMID: 33213394; PMCID: PMC7675397.
- Cao J, Tu WJ, Cheng W, Yu L, Liu YK, Hu X, Liu Q. Clinical Features and Short-term Outcomes of 102 Patients with Coronavirus Disease 2019 in Wuhan, China. Clin Infect Dis. 2020 Jul 28;71(15):748-755. doi: 10.1093/cid/ciaa243. PMID: 32239127; PMCID: PMC7184479.
- Parikh PA, Shah BV, Phatak AG, Vadnerkar AC, Uttekar S, Thacker N, Nimbalkar SM. COVID-19 Pandemic: Knowledge and Perceptions of the Public and Healthcare Professionals. Cureus. 2020 May 15;12(5):e8144. doi: 10.7759/cureus.8144. PMID: 32550063; PMCID: PMC7294885.
- Wolf MS, Serper M, Opsasnick L, O'Conor RM, Curtis L, Benavente JY, Wismer G, Batio S, Eifler M, Zheng P, Russell A, Arvanitis M, Ladner D, Kwasny M, Persell SD, Rowe T, Linder JA, Bailey SC. Awareness, Attitudes, and Actions Related to COVID-19 Among Adults With Chronic Conditions at the Onset of the U.S. Outbreak: A Cross-sectional Survey. Ann Intern Med. 2020 Jul 21;173(2):100-109. doi: 10.7326/M20-1239. Epub 2020 Apr 9. PMID: 32271861; PMCID: PMC7151355.
- Hsiao TC, Chuang HC, Griffith SM, Shui JC, Young LH. COVID-19: An aerosol’s point of view from expiration to transmission to viral-mechanism. Aerosol and Air Quality Research.2020;20(5):905-910. doi: 10.4209/aaqr.2020.04.0154.
- Reuben RC, Danladi MMA, Saleh DA, Ejembi PE. Knowledge, Attitudes and Practices Towards COVID-19: An Epidemiological Survey in North-Central Nigeria. J Community Health. 2021 Jun;46(3):457-470. doi: 10.1007/s10900-020-00881-1. PMID: 32638198; PMCID: PMC7338341.
- Yancy CW. COVID-19 and African Americans. JAMA. 2020 May 19;323(19):1891-1892. doi: 10.1001/jama.2020.6548. PMID: 32293639.
- Dyer O. Covid-19: Black people and other minorities are hardest hit in US. BMJ. 2020 Apr 14;369:m1483. doi: 10.1136/bmj.m1483. PMID: 32291262.
- Webb Hooper M, Nápoles AM, Pérez-Stable EJ. COVID-19 and Racial/Ethnic Disparities. JAMA. 2020 Jun 23;323(24):2466-2467. doi: 10.1001/jama.2020.8598. PMID: 32391864.
- Akalu Y, Ayelign B, Molla MD. Knowledge, Attitude and Practice Towards COVID-19 Among Chronic Disease Patients at Addis Zemen Hospital, Northwest Ethiopia. Infect Drug Resist. 2020 Jun 24;13:1949-1960. doi: 10.2147/IDR.S258736. PMID: 32612371; PMCID: PMC7322118.
- Bhutta ZA, Basnyat B, Saha S, Laxminarayan R. Covid-19 risks and response in South Asia. BMJ. 2020 Mar 25;368:m1190. doi: 10.1136/bmj.m1190. PMID: 32213488.
- Vince G. The world's largest refugee camp prepares for covid-19. BMJ. 2020 Mar 26;368:m1205. doi: 10.1136/bmj.m1205. PMID: 32217520.
- IEDCR. COVID-19. 2020. https://tinyurl.com/w4ypm7b2
- Ramphul K, Mejias SG. Coronavirus Disease: A Review of a New Threat to Public Health. Cureus. 2020 Mar 15;12(3):e7276. doi: 10.7759/cureus.7276. PMID: 32300496; PMCID: PMC7158591.
- Chen Y, Liu Q, Guo D. Emerging coronaviruses: Genome structure, replication, and pathogenesis. J Med Virol. 2020 Apr;92(4):418-423. doi: 10.1002/jmv.25681. Epub 2020 Feb 7. Erratum in: J Med Virol. 2020 Oct;92(10):2249. PMID: 31967327; PMCID: PMC7167049.
- Liu K, Chen Y, Lin R, Han K. Clinical features of COVID-19 in elderly patients: A comparison with young and middle-aged patients. J Infect. 2020 Jun;80(6):e14-e18. doi: 10.1016/j.jinf.2020.03.005. Epub 2020 Mar 27. PMID: 32171866; PMCID: PMC7102640.
- Rahman MS, Karamehic MA, Amrin M, Chowdhury AH, Mondol MdS, Haque U, Parveen AA. COVID-19 Epidemic in Bangladesh among rural and urban residents: An online cross-sectional survey of knowledge, attitudes, and practices. Epidemiologia. 2021;2:1–13. doi: 10.3390/epidemiologia2010001.
- Hossain MA, Jahid MIK, Hossain KMA, Walton LM, Uddin Z, Haque MO, Kabir MF, Arafat SMY, Sakel M, Faruqui R, Hossain Z. Knowledge, attitudes, and fear of COVID-19 during the Rapid Rise Period in Bangladesh. PLoS One. 2020 Sep 24;15(9):e0239646. doi: 10.1371/journal.pone.0239646. PMID: 32970769; PMCID: PMC7514023.
- Ogolodom MP, Mbaba AN, Alazigha N, Erondu OF, Egbe NO, Golden I, Ugwuanyi DC, Achi GI and Eke CM. Knowledge, Attitudes and Fears of Health Care Workers towards the Corona Virus Disease (COVID-19) Pandemic in South-South, Nigeria. Heal Sci J. 2020;Sp.Iss.1:002. doi:10.36648/1791-809X.S1.002.
- Zhu ZB, Zhong CK, Zhang KX, Dong C, Peng H, Xu T, Wang AL, Guo ZR, Zhang YH. [Epidemic trend of COVID-19 in Chinese mainland]. Zhonghua Yu Fang Yi Xue Za Zhi. 2020 Jun 6;54(6):620-624. Chinese. doi: 10.3760/cma.j.cn112150-20200222-00163. PMID: 32125133.
Content Alerts
SignUp to our
Content alerts.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.