Medicine Group. 2023 October 15;4(10):1412-1421. doi: 10.37871/jbres1811.
The Impact of COVID-19 Pandemic on Cardiovascular Diseases in Brazil
Gilberto Henrique NL Lopes1#, Joselene Beatriz S da Silva2#, Ronian S Carvalho1, Marcos Vinicius T Martins1, Santiago S Rocha1 and Stefan V de Oliveira3*
- Heart diseases
- Hospitalizations
- Healthcare services research
- Coronavirus infections
Abstract
Background: The novel coronavirus pandemic is an international public health emergency due to the high contagious potential of the virus on a global scale and, similarly to what happened globally, Brazilian authorities took measures to reduce its impact on the healthcare system, including social distancing. In this context of exhaustion of the system, it is worth questioning the situation of patients who need medical care for other diseases, such as the cardiovascular ones.
Objectives: Describe the changes in the epidemiological profile of hospitalizations cardiovascular diseases during the COVID-19 pandemic in Brazil.
Methods: Assessment of relative variations on the number of hospitalizations, associated average time, mortality rate and financial investments.
Results: After the beginning of the pandemic, there was reduction of 21.46% in hospitalizations, more accentuated in females and in the Northern region, and increase of 14.14% in mortality, of greater significance in the Midwestern region. In younger ages, mortality and permanence time presented more accentuated positive variations. In elective admissions, growth in mortality and in hospital expenses were more significant.
Conclusion: The pandemic impacted on cardiovascular diseases in a multifactorial way. The number of hospitalizations decreased, and the mortality rate increased, as efforts concentrated on moderate and severe cases. Therefore, there is a need for policies that minimize mid- and long-term impacts, as well as studies that investigate possible late complications of infections by the novel coronavirus.
Introduction
Recognized on March 11th 2020 by the World Health Organization (WHO), the COVID-19 (Coronavirus Disease 2019) pandemic is an international public health emergency due to the high contagious potential of the virus on a global scale. Initially identified in China at the end of 2019, where infected people had a clinical picture similar to a potentially lethal pneumonia, other countries began to record infections with the virus from January 2020. Brazil officially registered its first case on February 26th 2020 [1,2].
Despite having a lower mortality rate than other coronaviruses, the high transmissibility of COVID-19 poses a threat of collapsing the functioning of public healthcare systems in several countries due to its high demand for urgent treatment of complications. According to WHO data, on July 24th, 2020, the COVID-19 pandemic summed up 15,296,926 confirmed cases in 216 countries and 585,727 deaths. In Brazil, on the same date, there were 2,347,238 cases and 85,259 deaths [3]. As the same happened around the world, Brazil also took measures to reduce the impact on the healthcare system, including social distancing [2,4].
In the context of an exhausted healthcare system, social distancing and fear, it is worth questioning the situation of patients who need medical care for other diseases. Among them, cardiovascular diseases stand out, which in 2019 were responsible for 98,293 deaths and generated a cost of R$3,097,015,094.33 (approximately US$ 772,361,487.94) to SUS (Unified Healthcare System, in Portuguese), the Brazilian public healthcare system [5].
Additionally, considering Brazil’s status as a middle income country, the epidemiological profiles and prognostic expectations for cardiovascular illnesses present in significantly different profiles, which differ greatly from the scenario in high income countries [6]. Thus, changes in the pattern of statistical variation related to the treatment of patients with cardiovascular diseases can show how the pandemic context influences the way these patients seek and obtain healthcare, modifying, for example, the mortality rate, the amount and the average time of hospitalizations [5,7]. Moreover, such variations should be a warning for healthcare authorities to seek ways to avoid struggles in carrying out such care: Either by preventing that, when experiencing symptoms of these diseases, patients be afraid to seek care due to the risk of contamination by COVID-19 in healthcare facilities; or by preventing the collapse of the system from affecting the care of these patients. Therefore, this paper aims to describe the changes in the epidemiological profile of hospitalizations cardiovascular diseases during the COVID-19 pandemic in Brazil.
Materials and Methods
Study design
This study is epidemiological, descriptive and quantitative.
Data sources
We used secondary data referring to hospitalizations registered in Brazil, between the years 2018 and 2021, considering diseases of the circulatory system, as indicated in the Hospital Information System of the Unified Health System (SIH/SUS), which is available at the electronic address of the Department of Informatics of SUS (DATASUS) [8].
We analyzed diseases described in the Chapter IX of the International Statistical Classification of Diseases and Related Health Problems (ICD-10) [9], composed of chronic and acute rheumatic diseases, ischemic heart diseases, hypertensive and cerebrovascular diseases, diseases of the arteries, arterioles, capillaries, veins, vessels and lymph nodes, diseases of the pulmonary circulation and other diseases of the cardiovascular system. We included in the study all cases of hospitalizations for pathologies of the circulatory system in the country’s territory during the specified time period and excluded cases with missing information or whose care was given in foreign territories.
Statistical analysis
We evaluated the relative variations in the number of hospitalizations, associated mean time and mortality rate according to the profile of cases present in the aforementioned system, comparing the periods from January 2018 to December 2019 and January 2020 and December 2021. We based the design of this profile on the year and month of registration, state and region of all hospitalizations, regarding both the temporal and spatial distribution of cases in the national territory. Additionally, we used the demographic profile as distinctive parameters, analyzing data according to the hospitalizations form for gender (male or female), age (in years), and race/color (white, black, yellow, brown and indigenous, which are the most usual terms in Brazil, considering the country's wide mixed race context, which makes racial categorization such as European, African, Native American or Asian usually difficult to define).
Data collection took place through DATASUS File Transfer System and its organization and tabulation took place with the help of RStudio and Microsoft Office Excel software. In the first tool, we also carried out statistical analyzes, having calculated measures of dispersion, central tendency, and frequency for the study variables. In order to validate possible differences in these indicators, we performed Student's T tests for independent samples and Mann-Whitney U tests in cases in which the assumptions for parametric tests were not met. More specifically, in the calculations of case incidence, we considered prevalence ratios per 100,000 inhabitants, based on population estimates from the Brazilian demographic censuses from 2007 to 2019. The alpha level used for establishing statistical significance is 0.05.
Ethical considerations
Due to the use of secondary data of public nature and without nominal identification of the subjects, this study does not need the appreciation of the Research Ethics Committee, in accordance with what the resolution of the Brazilian National Health Council number 466, of December 12, 2012 [10], establishes, which regulates the guidelines for research involving human beings.
Results
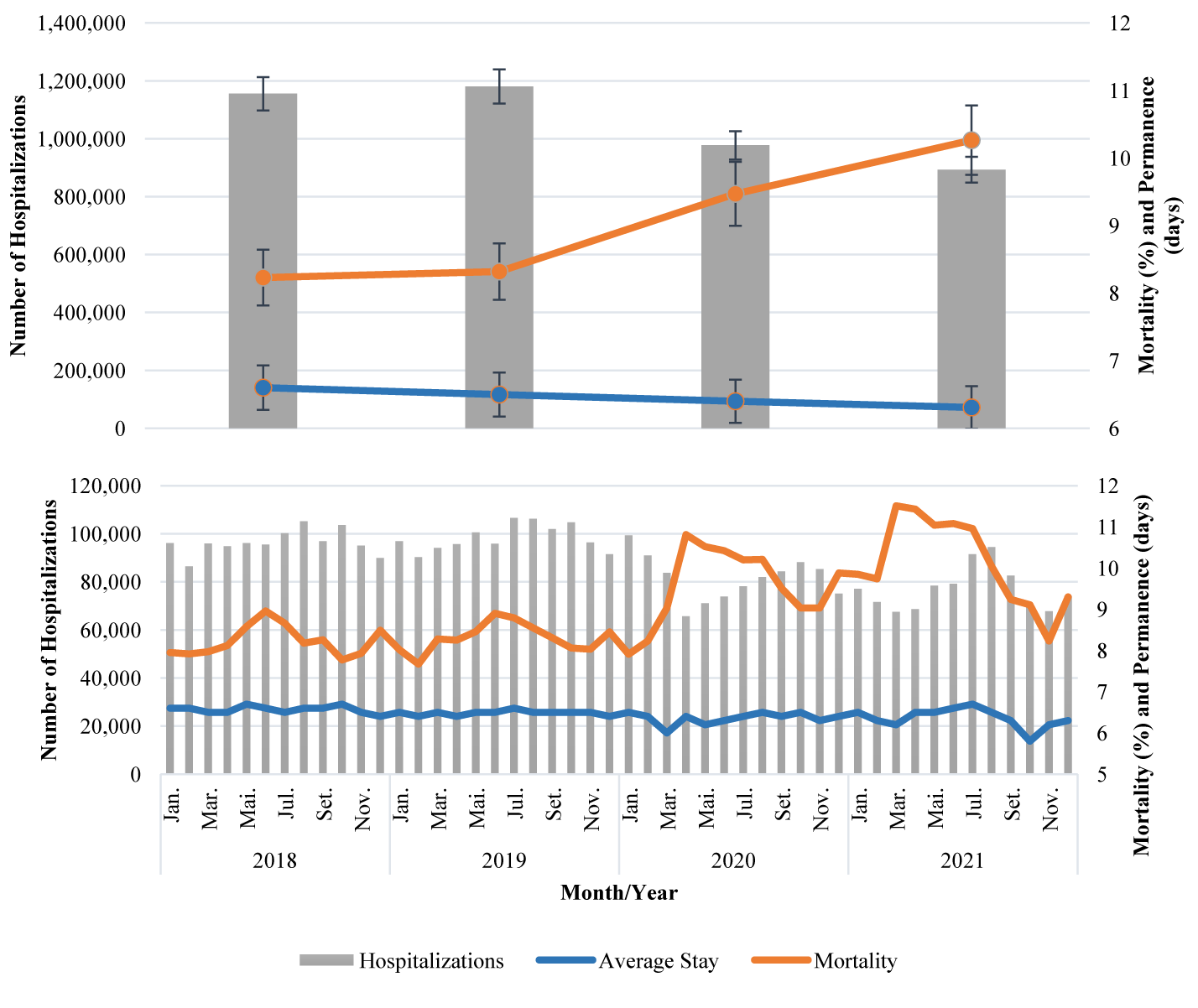
The average monthly hospitalizations recorded for the years 2020 and 2021 was 77,948 (±4.944), which is lower than the average of 97,336 (±2.134) recorded for the years 2018 and 2019. The average reduction observed per federation unit for the first and second semesters of those periods was 18.54% (±7.55) and 21.22% (±8.36), respectively, and 19.92% (±7.98) when considering the full period. With regard to the mortality rate, there was an upward trend in the values for 2020 and 2021 when compared to previous years. The monthly averages for these rates increased from 8.27% (±0.49) to 9.88% (±1.38).
Regarding the average length of stay, there was relative stability in the years analyzed, with no statistical differences between the values for the periods from 2018 to 2019 and 2020 to 2021 (p = 0.6322). The number of hospitalizations, average times and mortality rates according to month and year of occurrence are in figure 1.
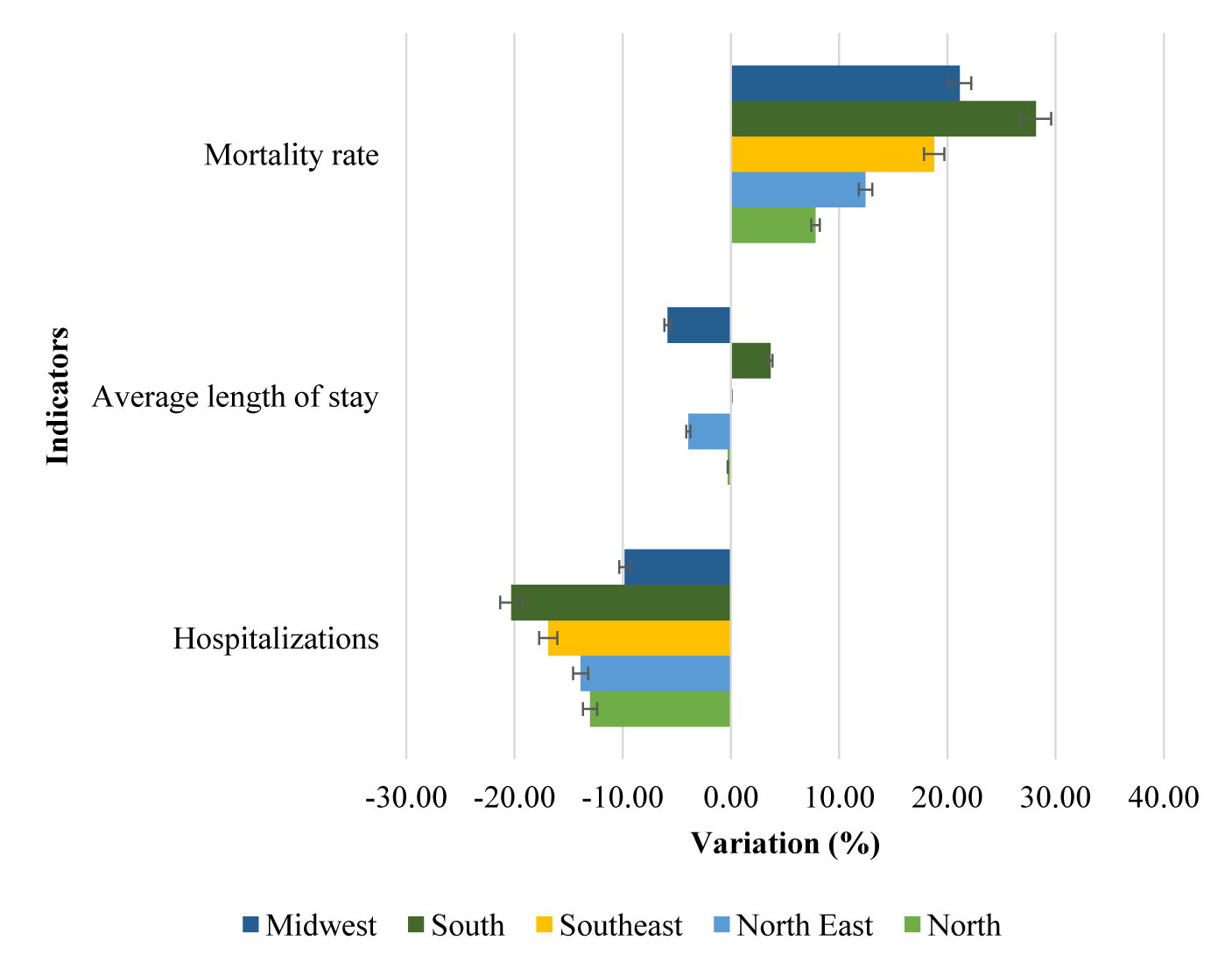
It was possible to notice the same trends in the national scenario, of decrease in the number of hospitalizations and increase in mortality in each of the macro-regions of the country, as shown in figure 2.
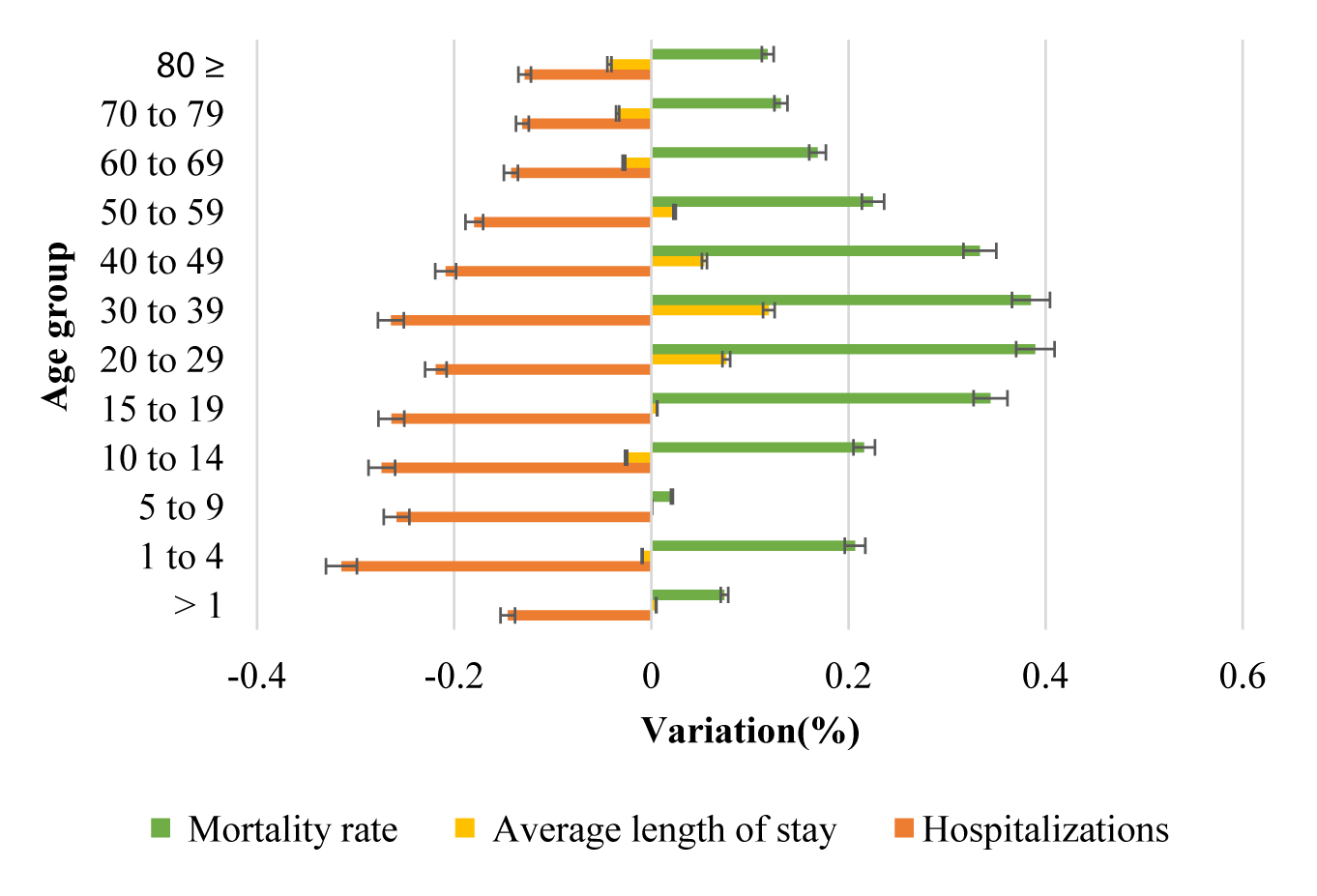
Regarding the distribution by sex, there was a more accentuated reduction in hospitalizations of females, 20.22% (±8.06), when compared to males, 12.64% (±5 .52). We observed no significant differences in the mean length of hospital stay and mortality rate. Considering the distribution of cases by age group, there was a smaller reduction in the number of hospitalizations with advancing age (p = 0.0209). For mortality rates and length of stay, we observed more substantial positive variations in individuals aged between 20 and 39 years (Figure 3). In addition, there was reduction in hospitalization in all age groups among children, with a greater reduction in the age group from 1 to 4 years, 31%. Regarding the mortality rate, there was general increase, with the highest one observed in the 10-14 age group, 21.6%. The average length of stay remained relatively unchanged, with a minimum decrease of 2.5% from 10 to 14 years. Moreover, there was no significant variation in the mean age of hospitalized individuals, which was 62.65 (± 5.24) years.
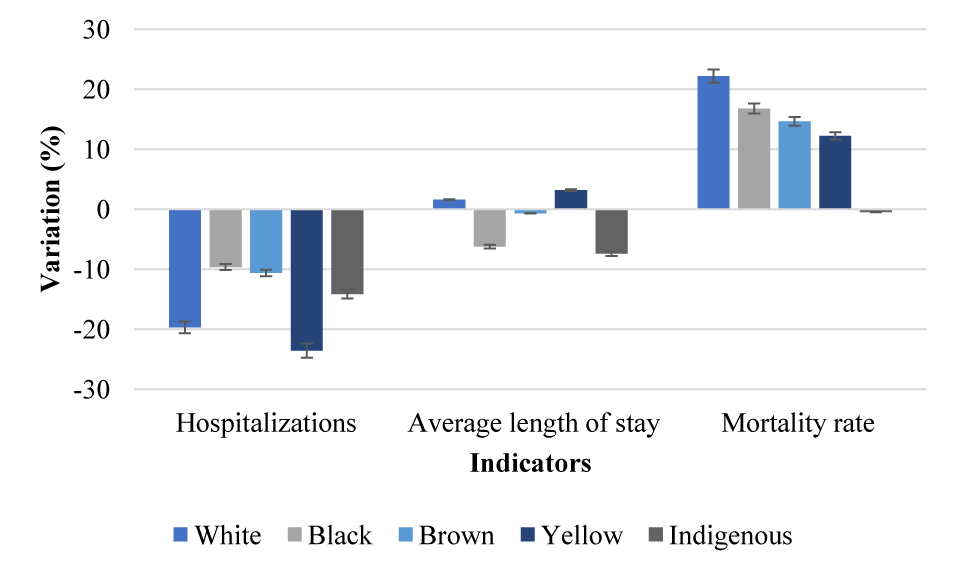
As for the analysis by ethnicity, the variations in the mortality rate, average length of stay and number of hospitalizations are in figure 4. It is important to note that the variations in the mortality rate for the indigenous population were not statistically different from zero (p = 0.5231).
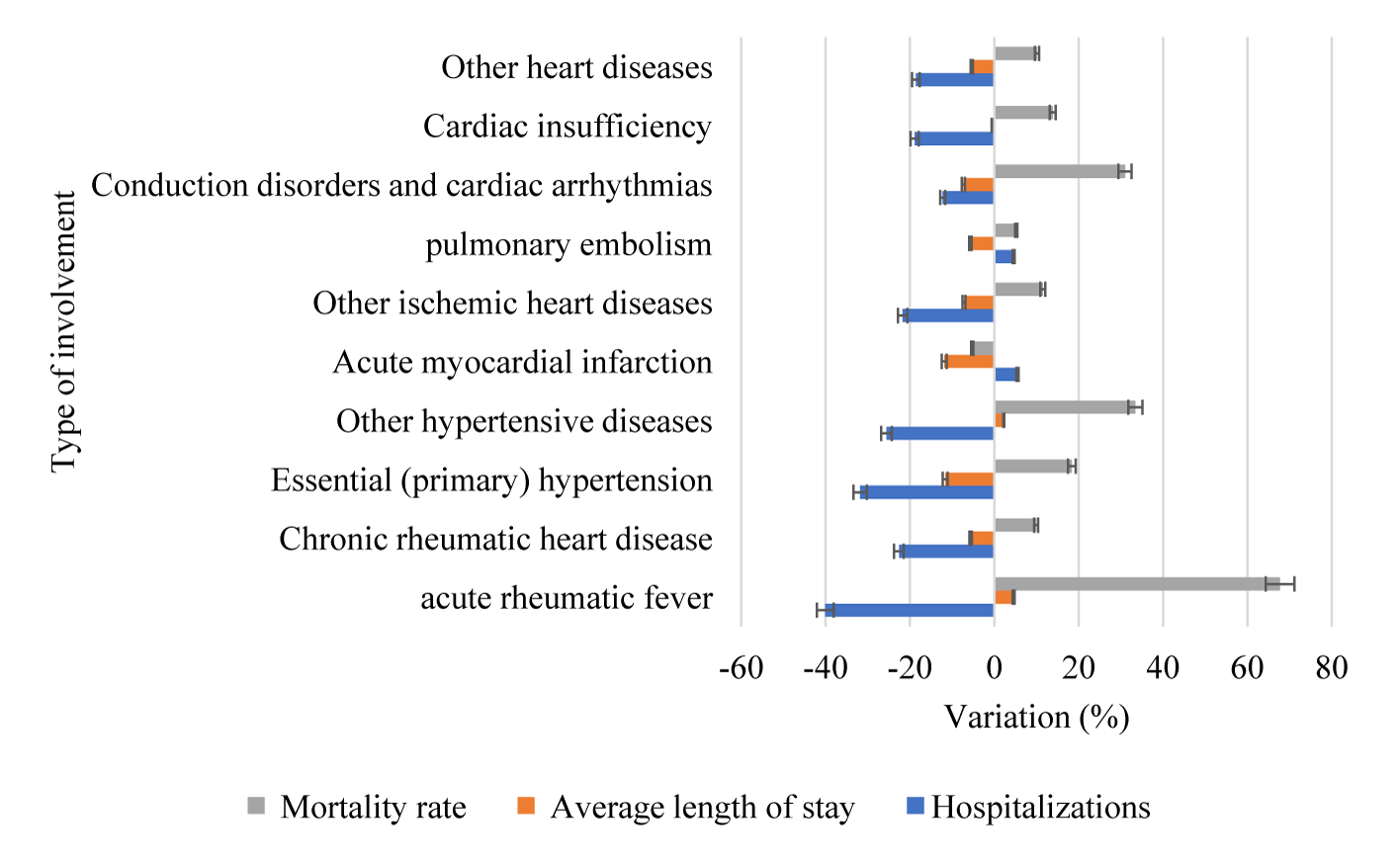
When we stratified the occurrences according to the type of cardiovascular disease, we noticed that, despite the generally observed trend of reduction in the number of cases, there was increase in hospitalizations for pulmonary embolism (p = 0.0214) and acute myocardial infarction (p = 0.0021). In figure 5 it is possible to observe in greater detail the study variables’ behavior according to the type of cardiovascular involvement.
The evaluation of the type of care provided indicated a more significant increase in the mortality rate, 49.51% (±3.08), and length of stay, 21.21% (±2.34), in cases of elective hospitalizations. As for the monthly averages of hospitalizations referring to elective cases, there was a reduction of 37.36% (±3.90). For urgent cases, these values became 12.50% (±7.03), 4.29 (±2.05) and 11.51 (±5.09).
Discussion
The average reduction observed for hospitalizations in the country was 19.92% (±7.98). The evaluation of data from the entire Brazilian territory shows important changes in the pattern of hospitalizations during the pandemic period, similar to those observed in other countries [11,12]. There was a significant reduction in the number of total hospitalizations, with a greater reduction in the number of admissions for female patients. Furthermore, despite the relative stability of the length of stay and the average age of the hospitalized subjects, there was a worrying increase in mortality among the youngest and the hospitalized patients for elective procedures.
Upon analyzing the decrease in the quantity of hospitalizations, the periods with its most expressive numbers coincided with the most serious periods of the pandemic in Brazil among the analyzed months [13]. Thus, it is necessary to highlight the multifactorial impact of the pandemic, both on individuals and on the entire healthcare system. The challenges arising from the reallocation of resources to mitigate the burden on the healthcare services [14], such as the reduction or suspension of elective surgeries [15], associated with patients' aversion to seeking hospital services for acute cardiovascular conditions [12,16], led to a scenario in which the profile of care was condensed into moderate to severe cases, which may explain the variations in the profiles of the variables studied here. It is also worth mentioning that telemedicine had a prominent place, spreading exponentially across the country, by enabling the management of chronic diseases and mild cases of COVID-19 remotely, thus reducing the number of face-to-face consultations. However, it should be noted that Brazil is a country with important barriers to its complete dissemination, since access to the internet and online consultation platforms is difficult when analyzing the less favored portions of the Brazilian population [17].
Considering the national data, one should, above all, take into account the medium- and long-term consequences of such a situation regarding the profile and severity of cases of cardiovascular diseases [12,16]. One remarkable finding is the data regarding Acute Rheumatic Fever Cardiac Disease cases, which showed both the largest increase in relative mortality rate and the largest decrease in hospitalizations. Considering the disease profile, which presents a significant correlation between low socioeconomic status and its incidence and severity [6], the data implicates a high impact of the worsening healthcare conditions during the pandemic period on the prevention, diagnosis and treatment of those conditions. Considering the magnitude of the observed effect, further studies on the epidemiological profile of Acute Rheumatic Fever and the application of additional strategies to cope with the worsening outcomes are deemed necessary and highly recommended by the authors.
In addition, we observe that the only diseases that had an increase in the number of hospitalizations were Acute Myocardial Infarction (AMI) and pulmonary embolism. Furthermore, SARS-CoV-2 virus has a pathophysiology intrinsically linked to coagulation disorders, correlated with the severity of the cases [18], and mechanisms of the inflammatory response during hypercytokinemia are associated with the activation of the coagulation cascade [19,20]. Moreover, COVID-19 is an independent risk factor for ischemic stroke [21] with a strong correlation with vascular occlusions of large vessels in young people [22], acute myocardial injuries and arrhythmias [23].
Furthermore, previous reports show that more than a quarter of the critically ill patients have some kind of cardiovascular disease with strong correlations between cardiovascular diseases and increased fatality rates among hospitalized covid-positive patients [24]. We believe that future studies will be able to analyze the specific impact of congenital heart diseases on the complication rates of COVID-19 within the Brazilian population, as studies with other populations have shown that this seems to have exerted an impact on covid-19 complication rates [25].
Despite that, the analysis of the number of hospitalizations per disease is subject to underreporting bias, not allowing us to infer whether the incidence of other diseases has decreased. Additionally, severe cases of COVID-19 are associated with chronic non-transmissible diseases such as diabetes [25,26] hypertension [25] and common medications used to treat cardiovascular conditions [27], which further impacts the reliability of inferring a correlation from the data alone. However, although the societal and organizational effects of the pandemic response add significant noise to the hospitalization data relative to the pre-pandemic data, the high correlation between cardiac conditions and cardiac risk factors in severe COVID-19 cases [24,28] indicates a relevant impact of such factors in the prognosis of COVID-19 infections. Therefore, the direct relations between COVID-19 and the variations of the number of hospitalizations per disease should be reviewed taking into account not only the statistical data and pathophysiology of both diseases, but also the behavioral patterns for treatment seeking and the distortions in the availability of medical service during the pandemic.
Regarding the different regions, we observe a general decrease in hospitalizations and increase in mortality in all regions, however with a mixed picture regarding the average length of stay. The data indicates a change in the pattern of hospitalizations and deaths as, from 1980 to 2017 [29,30] there was a statistical trend of reduction of general mortality and increase of cardiovascular hospitalizations. Additionally, it is worth noting the situation of the South macroregion, which was the only region to show an increase in the average length of stay. Furthermore, there is a heterogeneous distribution of data among the different regions [29-31] and, as the economic and socio-demographic conditions of a region are correlated to the incidence of cases of previous heart diseases and other chronic non-transmissible diseases [30] which impact the severe complications of COVID-19 infection, those variations could be reasonably expected.
However, it is necessary to highlight the biases of underreporting and limited coverage in the North and Northeast regions [31]. We specially emphasize the need for a careful examination of the information related to the North region, whose lower availability of doctors, hospital beds, and more limited healthcare system coverage during the pandemic [32], associated with the regional profile for cardiovascular diseases, are impactful factors that differentiate the region among the others.
Regarding the ethnic distribution, there was no statistically significant variation on the mortality rate of the indigenous population, which may be due to the small number of indigenous individuals hospitalized during the period (n = 750). Moreover, 29% of the country's indigenous population live in the North region and, in this region, the group is predominantly rural with about 78% of them living in non-urban areas [33]. Furthermore, this relative isolation from densely populated centers may correspond to a protective factor for the group, especially if one considers the role of COVID-19 as an aggravating factor for heart conditions.
Considering data from PNAD (National Household Sample Survey, in Portuguese) 2003, the incidence of heart disease in women corresponds to about 60% of the total [33]. Thus, having the most significant reduction in the number of hospitalizations been observed in the female population may indicate a lower severity of the symptoms despite the higher prevalence. Those findings are compatible with previous studies showing that men with COVID-19 infection have >50% higher risk of all-cause death, severe COVID-19 infection, or ICU admission than women, even adjusting for age and comorbidities [34]. There is a multitude of possible physiological mechanisms thought to underpin the discrepancy in outcomes, ranging from higher predisposition of older and low-testosterone men to develop severe forms of the infection [35] to the anti-inflammatory effects of the hormonal changes which occur during the female reproductive cycle and pregnancy [36], which are believed to attenuate the cytokine response and in turn reduce the severity of deleterious inflammatory effects in target tissues. However, further studies are needed before any conclusive statement can be made about causal relations between physiology and the disparity in prognosis.
Regarding age, the data shows that older individuals remained as the predominant age group affected since the start of the pandemic. It is worth noting the aging trend of the Brazilian population, as between the years 2010 and 2015 the population aged 65 or older increased by 22% [37]. According to data from PNAD 2003, occurrences of heart disease among the elderly are more substantial [33] and, due to the severity of the cases and associated comorbidities which are more frequent in this group [37], one can justify the lower variations in the numbers of hospitalizations in this age group. We observed a similar pattern in the children's age groups, since there was an overall reduction in hospitalizations of children, but with significant increase in mortality in the age groups from 1 to 4 years old and from 10 to 14 years old. The reduction in hospitalization rates could be seen as a sign that the COVID-19 infection has less repercussions in children, as seen in previous reports [38]. Nevertheless, the increase in mortality evidenced in the aforementioned age groups makes additional studies necessary.
Assessments of costs related to heart diseases in the country for the period from 2010 to 2015 indicated that 0.7% of the national GDP was allocated for this purpose, a very significant value as it represents 9.5% of all the healthcare expenditure of the country [35]. Considering the aging trend described for the Brazilian population and the predominance of such diseases in the elderly, this figure may increase in the upcoming years [35].
Nevertheless, the effects of the pandemic response measures on the population’s health should not be ignored - both due to deleterious effects on the individuals’ mental health [4] and due to changes in diet and physical activity habits [39]. Quarantine and social distancing present major challenges to the analysis of population health habits, in part due to a poor quality of information regarding factors such as physical activity at home, a point neglected in pre-existing guidelines [39]. Overall, increases in chronic conditions with negative impact on vascular health, such as stress and obesity, are likely to happen [39], and we should consider such factors when analyzing epidemiological data.
Conclusion
It is possible to observe that in the pandemic period the number of hospitalizations for cardiovascular diseases in Brazil decreased substantially, mainly in the second semester, whereas the mortality rate increased as the healthcare was concentrated in moderate and severe cases. With the exception of hospitalizations for AMI and pulmonary embolism, which increased, all hospitalizations for cardiovascular diseases decreased. The South region of the country had the greatest decrease in hospitalizations and the greatest increase in mortality. Regarding ethnicities, we observed no sole increase in the mortality of indigenous people. There was a more important increase in the mortality rate and length of elective hospitalizations. Thus, we highlight the need for the responses to public health measures aimed at the prevention and treatment of cardiovascular diseases to be guided by the particularities of each region, so that resources can be reallocated effectively.
Declarations
Data availability statement
The data accessed in this study can be consulted at the Department of Informatics of the Brazilian Unified Health System at this link http://tabnet.datasus.gov.br/cgi/deftohtm.exe?sih/cnv/niuf.def.
Acknowledgment
We thank the team from the Department of Collective Health of the Faculty of Medicine and Graduate Program in Health Sciences of the Federal University of Uberlândia who encouraged this research, providing the resources for this study to be developed.
Conflicts of interest
The authors declare no conflict of interest.
Author contributions
Conceptualization, G.H.N.L.L., J.B.S.S. and R.S.C.; methodology, M.V.T.M and S.V.O.; validation, SVO; formal analysis, M.V.T.M; original draft preparation, G.H.N.L.L., J.B.S.S., S.S.R. and R.S.C; writing-review and editing, MVTM, R.S.C. and SVO; supervision, SVO.
Funding
This research received no external funding.
References
- Bezerra ACV, Silva CEMD, Soares FRG, Silva JAMD. Factors associated with people's behavior in social isolation during the COVID-19 pandemic. Cien Saude Colet. 2020 Jun;25(suppl 1):2411-2421. Portuguese, English. doi: 10.1590/1413-81232020256.1.10792020. Epub 2020 Apr 23. PMID: 32520286.
- Aquino EML, Silveira IH, Pescarini JM, Aquino R, Souza-Filho JA, Rocha AS, Ferreira A, Victor A, Teixeira C, Machado DB, Paixão E, Alves FJO, Pilecco F, Menezes G, Gabrielli L, Leite L, Almeida MCC, Ortelan N, Fernandes QHRF, Ortiz RJF, Palmeira RN, Junior EPP, Aragão E, Souza LEPF, Netto MB, Teixeira MG, Barreto ML, Ichihara MY, Lima RTRS. Social distancing measures to control the COVID-19 pandemic: potential impacts and challenges in Brazil. Cien Saude Colet. 2020 Jun;25(suppl 1):2423-2446. English, Portuguese. doi: 10.1590/1413-81232020256.1.10502020. Epub 2020 Apr 22. PMID: 32520287.
- Coronavírus Brasil. Painel Coronavírus. 2020.
- Ornell F, Schuch JB, Sordi AO, Kessler FHP. "Pandemic fear" and COVID-19: mental health burden and strategies. Braz J Psychiatry. 2020;42(3):232-235. doi: 10.1590/1516-4446-2020-0008. Epub 2020 Apr 3. Erratum in: Braz J Psychiatry. 2020;42(3):333. PMID: 32267343; PMCID: PMC7236170.
- Ministério da Saúde (BR). DATASUS. Morbidade hospitalar do SUS - por local de residência - Brasil: óbitos segundo ano/mês processamento capítulo cid-10: ix. doenças do aparelho circulatório período: 2019. Óbitos segundo Ano/mês processamento Capítulo CID-10: IX. Doenças do aparelho circulatório. Brasília: Ministério da Saúde. 2020.
- Figueiredo ET, Azevedo L, Rezende ML, Alves CG. Rheumatic Fever: A Disease without Color. Arq Bras Cardiol. 2019 Jul 29;113(3):345-354. doi: 10.5935/abc.20190141. PMID: 31365604; PMCID: PMC6882402.
- Bitar H, Alismail S. The role of eHealth, telehealth, and telemedicine for chronic disease patients during COVID-19 pandemic: A rapid systematic review. Digit Health. 2021 Apr 19;7:20552076211009396. doi: 10.1177/20552076211009396. PMID: 33959378; PMCID: PMC8060773.
- Ministério da Saúde (BR). DATASUS: Informações de Saúde, Epidemiológicas e Morbidade: Banco de dados. Brasília. In: Ministério da Saúde; 2020.
- WHO. ICD-10 Version. 2016.
- Ministério da Saúde (BR). Resolução nº 466, de 12 de dezembro de 2012. Diretrizes e normas regulamentadoras de pesquisa envolvendo seres humanos. Diário Oficial da União. 2012.
- Zuin M, Mugnai G, Zamboni A, Zakja E, Valle R, Turiano G, Themistoclakis S, Scarpa D, Saccà S, Roncon L, Rizzetto F, Purita P, Polo A, Pantano I, Mugnolo A, Molon G, Meneghin S, Mancuso D, Lia M, Grassi G, Cutolo A, Chirillo F, Bozzini P, Bonapace S, Anselmi M, Rigatelli G, Bilato C. Decline of Admission for Acute Coronary Syndromes and Acute Cardiovascular Conditions during COVID-19 Pandemic in Veneto Region. Viruses. 2022 Aug 30;14(9):1925. doi: 10.3390/v14091925. PMID: 36146731; PMCID: PMC9502380.
- Metzler B, Siostrzonek P, Binder RK, Bauer A, Reinstadler SJ. Decline of acute coronary syndrome admissions in Austria since the outbreak of COVID-19: the pandemic response causes cardiac collateral damage. Eur Heart J. 2020 May 14;41(19):1852-1853. doi: 10.1093/eurheartj/ehaa314. PMID: 32297932; PMCID: PMC7184486.
- Ministério da Saúde (BR). Centro de operações de emergência em saúde pública| doença pelo Coronavírus 2019 (COE-COVID19). Boletim 17. Brasília: Ministério da Saúde. 2020.
- Emanuel EJ, Persad G, Upshur R, Thome B, Parker M, Glickman A, Zhang C, Boyle C, Smith M, Phillips JP. Fair Allocation of Scarce Medical Resources in the Time of Covid-19. N Engl J Med. 2020 May 21;382(21):2049-2055. doi: 10.1056/NEJMsb2005114. Epub 2020 Mar 23. PMID: 32202722.
- Diaz A, Sarac BA, Schoenbrunner AR, Janis JE, Pawlik TM. Elective surgery in the time of COVID-19. Am J Surg. 2020 Jun;219(6):900-902. doi: 10.1016/j.amjsurg.2020.04.014. Epub 2020 Apr 16. PMID: 32312477; PMCID: PMC7161516.
- Moroni F, Gramegna M, Ajello S, Beneduce A, Baldetti L, Vilca LM, Cappelletti A, Scandroglio AM, Azzalini L. Collateral Damage: Medical Care Avoidance Behavior Among Patients With Myocardial Infarction During the COVID-19 Pandemic. JACC Case Rep. 2020 Aug;2(10):1620-1624. doi: 10.1016/j.jaccas.2020.04.010. Epub 2020 Apr 23. PMID: 32835261; PMCID: PMC7252183.
- Camilo VC de O, Souto YS, Zavan N de O, Cardoso FR de O, Santos VA, Martins Machado A, Oda JY. Telemedicina e fatores limitantes para seu exercício no Brasil e no mundo durante a pandemia de Covid-19. In: Uma revisão integrativa. CONJ. 2021;21(6):866-82.
- Zhu J, Pang J, Ji P, Zhong Z, Li H, Li B, Zhang J, Lu J. Coagulation dysfunction is associated with severity of COVID-19: A meta-analysis. J Med Virol. 2021 Feb;93(2):962-972. doi: 10.1002/jmv.26336. Epub 2020 Oct 14. PMID: 32706396; PMCID: PMC7404826.
- Giannis D, Ziogas IA, Gianni P. Coagulation disorders in coronavirus infected patients: COVID-19, SARS-CoV-1, MERS-CoV and lessons from the past. J Clin Virol. 2020 Jun;127:104362. doi: 10.1016/j.jcv.2020.104362. Epub 2020 Apr 9. PMID: 32305883; PMCID: PMC7195278.
- Elkazzaz M, Ahmed A, Abo-Amer YE, Hydara T, Haikal A, Razek DNAE, Eltayb WA, Wang X, Karpiński TM, Hamza D, Jabbar B, Shamkh IM. In Silico Discovery of GPCRs and GnRHRs as Novel Binding Receptors of SARS-CoV-2 Spike Protein Could Explain Neuroendocrine Disorders in COVID-19. Vaccines (Basel). 2022 Sep 8;10(9):1500. doi: 10.3390/vaccines10091500. PMID: 36146578; PMCID: PMC9504287.
- Belani P, Schefflein J, Kihira S, Rigney B, Delman BN, Mahmoudi K, Mocco J, Majidi S, Yeckley J, Aggarwal A, Lefton D, Doshi AH. COVID-19 Is an Independent Risk Factor for Acute Ischemic Stroke. AJNR Am J Neuroradiol. 2020 Aug;41(8):1361-1364. doi: 10.3174/ajnr.A6650. Epub 2020 Jun 25. PMID: 32586968; PMCID: PMC7658882.
- Majidi S, Fifi JT, Ladner TR, Lara-Reyna J, Yaeger KA, Yim B, Dangayach N, Oxley TJ, Shigematsu T, Kummer BR, Stein LK, Weinberger J, Fara MG, De Leacy R, Dhamoon MS, Tuhrim S, Mocco J. Emergent Large Vessel Occlusion Stroke During New York City's COVID-19 Outbreak: Clinical Characteristics and Paraclinical Findings. Stroke. 2020 Sep;51(9):2656-2663. doi: 10.1161/STROKEAHA.120.030397. Epub 2020 Jul 31. PMID: 32755349; PMCID: PMC7434004.
- Bansal M. Cardiovascular disease and COVID-19. Diabetes Metab Syndr. 2020 May-Jun;14(3):247-250. doi: 10.1016/j.dsx.2020.03.013. Epub 2020 Mar 25. PMID: 32247212; PMCID: PMC7102662.
- Clerkin KJ, Fried JA, Raikhelkar J, Sayer G, Griffin JM, Masoumi A, Jain SS, Burkhoff D, Kumaraiah D, Rabbani L, Schwartz A, Uriel N. COVID-19 and Cardiovascular Disease. Circulation. 2020 May 19;141(20):1648-1655. doi: 10.1161/CIRCULATIONAHA.120.046941. Epub 2020 Mar 21. PMID: 32200663.
- Sabatino J, Di Salvo G, Calcaterra G, Bassareo PP, Oreto L, Cazzoli I, Calabrò MP, Guccione P, Gatzoulis MA; Congenital Heart Disease Working Group of the Italian Society of Cardiology (SIC). Adult congenital heart disease: Special considerations for COVID-19 and vaccine allocation/prioritization. Int J Cardiol Congenit Heart Dis. 2021 Aug;4:100186. doi: 10.1016/j.ijcchd.2021.100186. Epub 2021 Jun 16. PMID: 35360449; PMCID: PMC8206548.
- Fang L, Karakiulakis G, Roth M. Are patients with hypertension and diabetes mellitus at increased risk for COVID-19 infection? Lancet Respir Med. 2020 Apr;8(4):e21. doi: 10.1016/S2213-2600(20)30116-8. Epub 2020 Mar 11. Erratum in: Lancet Respir Med. 2020 Jun;8(6):e54. PMID: 32171062; PMCID: PMC7118626.
- Brito VP, Carrijo AMM, Oliveira SV. Associação da diabetes mellitus com a gravidade da COVID-19 e seus potenciais fatores mediadores: Uma revisão sistemática. Revista Thema. 2020; 18:204-217. doi: 10.15536/thema.V18.Especial.2020.204-217.1820.
- Li J, Wang X, Chen J, Zhang H, Deng A. Association of Renin-Angiotensin System Inhibitors With Severity or Risk of Death in Patients With Hypertension Hospitalized for Coronavirus Disease 2019 (COVID-19) Infection in Wuhan, China. JAMA Cardiol. 2020 Jul 1;5(7):825-830. doi: 10.1001/jamacardio.2020.1624. Erratum in: JAMA Cardiol. 2020 Aug 1;5(8):968. PMID: 32324209; PMCID: PMC7180726.
- Guimarães RM, Andrade SS, Machado EL, Bahia CA, Oliveira MM, Jacques FV. Diferenças regionais na transição da mortalidade por doenças cardiovasculares no Brasil, 1980 a 2012 [Regional differences in cardiovascular mortality transition in Brazil, 1980 to 2012]. Rev Panam Salud Publica. 2015 Feb;37(2):83-9. Portuguese. PMID: 25915012.
- Malta DC, Teixeira R, Oliveira GMM, Ribeiro ALP. Cardiovascular Disease Mortality According to the Brazilian Information System on Mortality and the Global Burden of Disease Study Estimates in Brazil, 2000-2017. Arq Bras Cardiol. 2020 Aug 28;115(2):152-160. English, Portuguese. doi: 10.36660/abc.20190867. PMID: 32696855; PMCID: PMC8384283.
- Figueiredo FSF, Rodrigues TFCDS, Rêgo ADS, Andrade L, Oliveira RR, Radovanovic CAT. Distribution and spatial autocorrelation of the hospitalizations for cardiovascular diseases in adults in Brazil. Rev Gaucha Enferm. 2020 Jun 12;41:e20190314. English, Portuguese. doi: 10.1590/1983-1447.2020.20190314. PMID: 32555957.
- Mendonça FD, Rocha SS, Pinheiro DLP, Pimenta DL, Oliveira SV. Região norte do Brasil e a pandemia de COVID-19: Análise socioeconômica e epidemiológica: J Health NPEPS. 2020;5(1):20-37.
- Instituto Brasileiro de Geografia e Estatística (IBGE). Pesquisa nacional por amostra de domicílios. Rio de Janeiro: IBGE. 2016.
- Kragholm K, Andersen MP, Gerds TA, Butt JH, Østergaard L, Polcwiartek C, Phelps M, Andersson C, Gislason GH, Torp-Pedersen C, Køber L, Schou M, Fosbøl EL. Association Between Male Sex and Outcomes of Coronavirus Disease 2019 (COVID-19)-A Danish Nationwide, Register-based Study. Clin Infect Dis. 2021 Dec 6;73(11):e4025-e4030. doi: 10.1093/cid/ciaa924. PMID: 32634827; PMCID: PMC7454435.
- Siqueira ASE, Siqueira-Filho AG, Land MGP. Analysis of the Economic Impact of Cardiovascular Diseases in the Last Five Years in Brazil. Arq Bras Cardiol. 2017 Jul;109(1):39-46. doi: 10.5935/abc.20170068. Epub 2017 Jun 1. PMID: 28591251; PMCID: PMC5524474.
- Papadopoulos V, Li L, Samplaski M. Why does COVID-19 kill more elderly men than women? Is there a role for testosterone? Andrology. 2021 Jan;9(1):65-72. doi: 10.1111/andr.12868. Epub 2020 Aug 5. PMID: 32681716; PMCID: PMC7404939.
- Berhan Y. What immunological and hormonal protective factors lower the risk of COVID-19 related deaths in pregnant women? J Reprod Immunol. 2020 Nov;142:103180. doi: 10.1016/j.jri.2020.103180. Epub 2020 Jul 18. PMID: 32739645; PMCID: PMC7368414.
- Rosa MFP, Silva WNT, Baccega TM, Castro IB, Oliveira SV. Síndrome respiratória aguda grave em pacientes pediátricos no contexto da pandemia: Uma análise epidemiológica do Brasil. Rev Ped SOPERJ. 2021;21(2):62-67. doi:10.31365/issn.2595-1769.v21i2p62-67.
- Mattioli AV, Sciomer S, Cocchi C, Maffei S, Gallina S. Quarantine during COVID-19 outbreak: Changes in diet and physical activity increase the risk of cardiovascular disease. Nutr Metab Cardiovasc Dis. 2020 Aug 28;30(9):1409-1417. doi: 10.1016/j.numecd.2020.05.020. Epub 2020 May 30. PMID: 32571612; PMCID: PMC7260516.
Content Alerts
SignUp to our
Content alerts.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.