> Medicine Group. 2021 June 01;2(6):425-428. doi: 10.37871/jbres1253.
Pneumocystis Jirovecii Pneumonia as a Sequela of COVID-19
Syed Muhammad Zubair1, Hamid Hussain Muhammad Zaid2 and Shahzad Talha1*
2Medical Student at Aga Khan Medical College, Karachi, Pakistan
- PCP
- Steroids
- Tocilizumab
- Bronchoscopy
- Sequelae
Abstract
A 71 years old male came to the hospital with the complaint of cough and fever since 7 days. He was diagnosed with severe COVID pneumonia and was managed with steroids and tocilizumab. He was discharged on steroids and came after 20 days with complaints of worsening shortness of breath and hypoxia. Bronchoscopy and bronchoalveolar lavage was done which showed positive PCR for Pneumocystis Jirovecii Pneumonia (PCP). Patient was started on co-trimoxazole and steroids after which he showed remarkable improvement. This is one of the rare cases in which patient developed PCP as a sequelae of COVID-19.
Introduction
Since the start of 2020, the whole world has been affected by one of the worst pandemics of all times. This pandemic continues to cripple the lives of patients during the infection and even after the infection has been cured. As more and more people are being cured, we now are stepping in an era where we will see post-COVID complications which can be infectious like COVID-19 associated pulmonary aspergillosis and non-infectious including myopathies, neuropathies and other neurological manifestations [1-3]. We present a case of an elderly gentleman who was treated with severe COVID pneumonia and then again presented after 20 days of his discharge with cough, worsening shortness of breath and hypoxia. Bronchoalveolar lavage was done which showed positive PCP PCR. This is one of the rarest case in literature in which PCP was seen as a sequelae of COVID-19 pneumonia.
Case Presentation
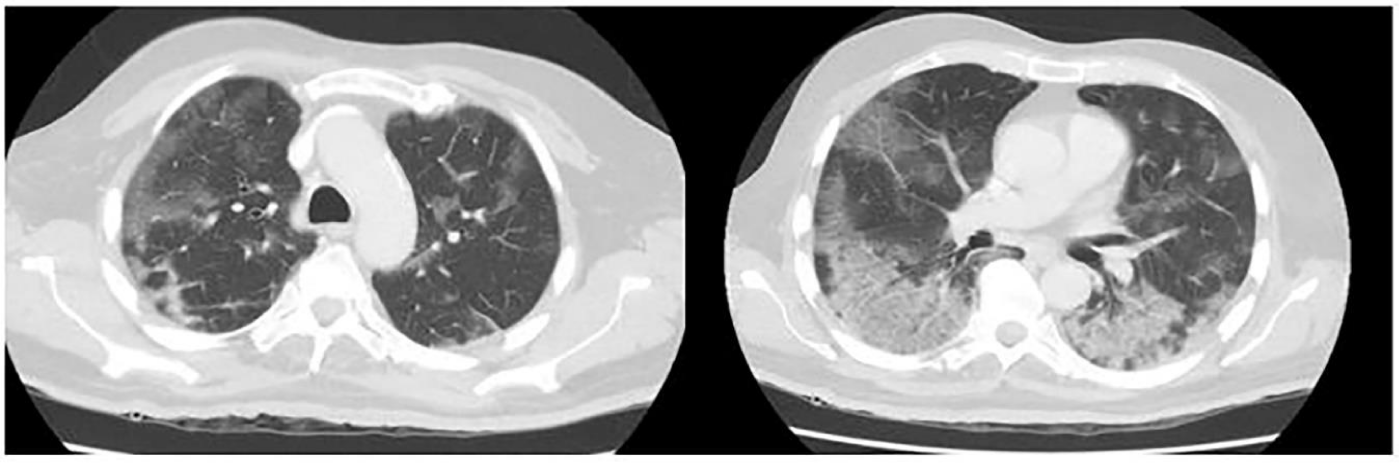
A 71 year old male with known co-morbidities of hypertension and diabetes mellitus presented to the emergency department with cough and fever. He developed these symptoms one week prior to presentation and were becoming worse. His cough was productive in nature and fever was fluctuating. Considering the on-going pandemic and alarming symptoms the patient had SARSCoV-2 RNA real time PCR done which was reported as positive. He was subsequently admitted. His complete blood count showed hemoglobin of 12.1 g/dl (normal 12.3-16.6 g/dl), white blood cell count of 6.4 x 109/L (normal 4.8-11.3 x 109/L) and platelets of 203 x 109/L (154-433 x 109/L). Serum ferritin and lactate dehydrogenase levels were 1735 ng/ml (normal 22-322 ng/ml) and 495 I.U/L (normal 120-246 I.U/L) respectively. C-reactive protein was 158 mg/L (normal 0 -10 mg/L) and d-dimer was 1.2 mg/L (normal <0.5 mg/L). The patient was managed in the hospital as severe COVID-19 pneumonia. Computed tomography scan of chest was done which showed patchy areas of ground glass opacities with peripheral predominance (Figure 1). He required oxygen and non-invasive ventilation. During his stay, he received two doses of Tocilizumab injection (600 mg each) and intravenous methylprednisolone 40 mg thrice a day for 11 days. During hospital stay, his conidition improved and he was discharged on 13th day of admission. Since the patient was hypoxic requiring 1-2 liters of supplemental oxygen and CT chest showed ground glass opacities with patchy consolidation hence the patient was discharged on oral prednisolone 20 mg twice a day (planned to be tapered on clinic visits). On discharge, patient’s oxygen requirement reduced to 1-2 liters, his serum (1,3)-b-D-glucan and galactomannan levels were within normal limits and there was clinical and radiographical improvement.
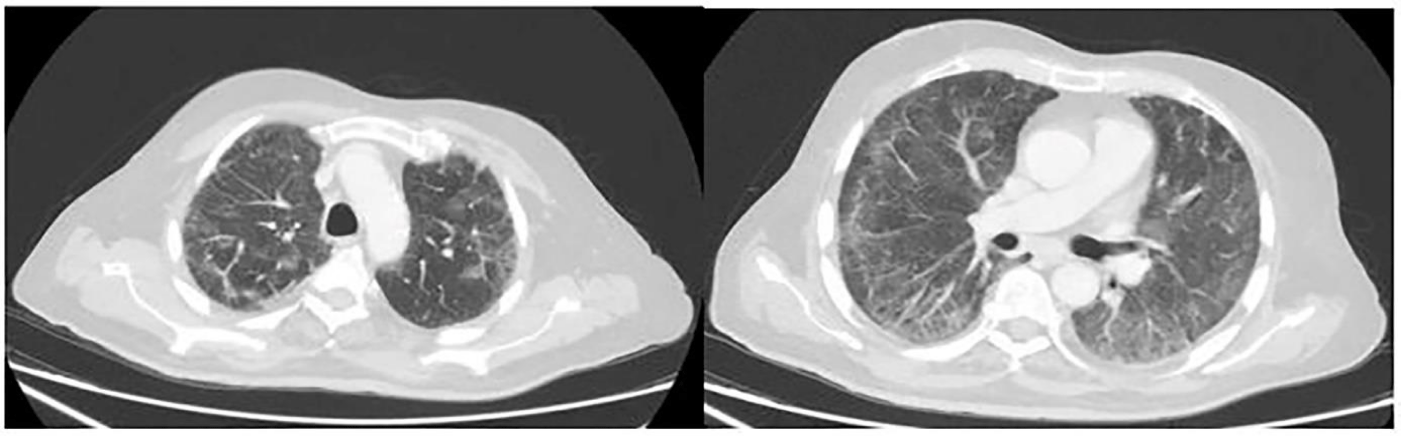
The patient returned to the emergency department after 20 days of his discharge due to worsening hypoxia and severe shortness of breath. At this time his steroids were tapered to 10 mg once a day. His vitals on presentation were: blood pressure 115/62 mmHg, heart Rate 76 beats per minute, respiratory rate 17 breaths per minute and oxygen saturations of 86% on room air which improved to 95% on 5 L/min of supplemental oxygen. Due to his worsening symptoms he was admitted. Baseline blood work up was done on admission which provided no clinically significant findings. SARS CoV-2 RNA real time PCR was negative twice. Serum (1,3)-b-D-glucan levels and galactomannan test were ordered. Serum (1,3)-b-D-glucan levels were reported as 252.264 pg/ml( Negative: <60 pg/ml and Positive: >80 pg/ml) and galactomannan was 0.141 (normal <0.5). A chest CT scan with contrast was ordered which showed patchy areas of ground glass haziness, diffusely scattered, which had a predominance for the sub pleural location and progression in the upper lobes. There was no evidence of pulmonary embolism (Figure 2). Due to the abnormal chest CT findings and persistent hypoxia, bronchoscopy and Bronchoalveolar Lavage (BAL) was done to rule out infectious causes. Gram stain and cultures of BAL including bacterial, fungal and tuberculosis were negative for any infections. PCP PCR came out to be positive. HIV serology was then also sent which came out to be negative.
Patient was started on co-trimoxazole and steroids as per PCP regimen. His condition gradually improved and he was discharged home with clinic follow up. Patient was followed up in clinic after a week of his discharge. He showed clinical improvement. He was maintaining saturations on room air.
Discussion
COVID-19 has taken the world by surprise. The management of COVID-19 is rapidly evolving with new literature and new trials coming at a rapid pace. However, with all the variety of drugs that we are using, we might see some unanticipated side effects and complications attributed to these drugs. In some instances, like in our case, multiple drugs can have a synergistic effect in the development and exacerbation of a complication. Our patient was diagnosed as post-COVID-19 PCP, which is currently an underestimated and underrated complication of COVID-19.
The early literature from Wuhan on COVID-19 have reported the development of fungal and bacterial co-infections in such patients [4]. Multiple bacterial infections and fungal infections like pulmonary aspergillosis have been reported in other viral infections like influenza [5,6].
COVID-19 Associated Pulmonary Aspergillosis (CAPA) is emerging as one of the recognized complication of COVID-19. Multiple studies are emphasizing on the fact that patients with severe COVID-19 pneumonia should be screened for pulmonary aspergillosis and soon it might be considered as one of the known infections infecting patients with COVID-19 [3,7,8]. Co-infection of COVID-19 and PCP have also been documented in literature [9].
We believe that in our case, post-COVID PCP was caused by a combination of steroids and tocilizumab. PCP can appear with a constellation of symptoms as seen in COVID-19. They both can appear with fever, dyspnea and fatigue. Additionally, bilateral ground glass opacities will be observed in both diseases. PCP can be due to different risk factors, but immunosuppression remains the main risk factor causing PCP [10]. With the advent of HIV retroviral therapy and subsequent PCP prophylaxis the incidence of PCP is decreasing substantially in this population. However, as more treatment guidelines are including an immunosuppressive agents to their regimes the incidence of PCP has increased in these patients [11]. It has been well documented that PCP can occur after a course of corticosteroid therapy, with one study finding that amongst 128 PCP cases around 87% were administered corticosteroids or other immunosuppressive therapies, prior to developing PCP. Similarly, our patient also has a history of long term steroid intake which can be an important risk factor for developing PCP. Apart from the steroid usage, the patient was given two doses of injectable tocilizumab as a treatment of Cytokine Release Syndrome in COVID-19 which is readily being used as a treatment modality as described in certain studies [12-14]. Tocilizumab is a humanized IL-6 antibody used mainly for rheumatoid arthritis, Giant Cell arteritis, systemic juvenile idiopathic arthritis and recently was being used in the management of COVID-19. A study found that serious infections occurred in about 8.5% of patients receiving tocilizumab monotherapy [15]. Another study from Japan also highlights the risk profile of tocilizumab (and other biologic agents) and development of PCP. The study found that amongst the 26 valid participants (being treated with tocilizumab and other biologic agents) 23 had contracted PCP [16]. In a clinical trial on tocilizumab 20 cases of invasive fungal infections were reported. Amongst them 1 of the cases was PCP and notably occurred with the low dose (4 mg/kg) injection [17]. All these studies on tocilizumab were done in the context of rheumatoid arthritis and we are mostly unaware of opportunistic infections in patients with COVID-19 treated with tocilizumab. Hence, in patients COVID-19 the risk of contracting PCP can be much higher. Further studies are necessary to highlight this risk.
Conclusion
COVID-19 sequelae is one of the underestimated entity at present. Even after the cure of acute infection, patient can present with infective and non-infective complications. Opportunistic infections like PCP should be one of the differential diagnosis in patients presenting with cough and hypoxia after COVID-19 especially if they have received steroids and IL-6 inhibitors like tocilizumab. PCP prophylaxis should be considered in patients recovering from COVID-19 who have received both steroids and tocilizumab. Serum (1,3)-b-D-glucan levels should be checked in patients with COVID-19 when there is a suspicion of co-infection. Early diagnosis can facilitate management and prevent fatal outcomes.
References
- Candan SA, Elibol N, Abdullahi A. Consideration of prevention and management of long-term consequences of post-acute respiratory distress syndrome in patients with COVID-19. Physiother Theory Pract. 2020 Jun;36(6):663-668. doi: 10.1080/09593985.2020.1766181. Epub 2020 May 18. PMID: 32419564.
- Lahiri D, Ardila A. COVID-19 Pandemic: A Neurological Perspective. Cureus. 2020 Apr 29;12(4):e7889. doi: 10.7759/cureus.7889. PMID: 32489743; PMCID: PMC7255551.
- Nasir N, Farooqi J, Mahmood SF, Jabeen K. COVID-19-associated pulmonary aspergillosis (CAPA) in patients admitted with severe COVID-19 pneumonia: An observational study from Pakistan. Mycoses. 2020 Aug;63(8):766-770. doi: 10.1111/myc.13135. Epub 2020 Jul 18. PMID: 32585069; PMCID: PMC7361517.
- Chen N, Zhou M, Dong X, Qu J, Gong F, Han Y, Qiu Y, Wang J, Liu Y, Wei Y, Xia J, Yu T, Zhang X, Zhang L. Epidemiological and clinical characteristics of 99 cases of 2019 novel coronavirus pneumonia in Wuhan, China: a descriptive study. Lancet. 2020 Feb 15;395(10223):507-513. doi: 10.1016/S0140-6736(20)30211-7. Epub 2020 Jan 30. PMID: 32007143; PMCID: PMC7135076.
- Zhou P, Liu Z, Chen Y, Xiao Y, Huang X, Fan XG. Bacterial and fungal infections in COVID-19 patients: A matter of concern. Infect Control Hosp Epidemiol. 2020 Sep;41(9):1124-1125. doi: 10.1017/ice.2020.156. Epub 2020 Apr 22. PMID: 32317036; PMCID: PMC7184139.
- Rijnders BJA, Schauwvlieghe AFAD, Wauters J. Influenza-Associated Pulmonary Aspergillosis: A Local or Global Lethal Combination? Clin Infect Dis. 2020 Oct 23;71(7):1764-1767. doi: 10.1093/cid/ciaa010. PMID: 31905234; PMCID: PMC7583400.
- Bruno G, Fabrizio C, Buccoliero GB. COVID-19-associated pulmonary aspergillosis: adding insult to injury. Lancet Microbe. 2020 Jul;1(3):e106. doi: 10.1016/S2666-5247(20)30063-X. Epub 2020 Jul 3. PMID: 32835340; PMCID: PMC7333985.
- Alanio A, Dellière S, Fodil S, Bretagne S, Mégarbane B. Prevalence of putative invasive pulmonary aspergillosis in critically ill patients with COVID-19. Lancet Respir Med. 2020 Jun;8(6):e48-e49. doi: 10.1016/S2213-2600(20)30237-X. Epub 2020 May 20. PMID: 32445626; PMCID: PMC7239617.
- Menon AA, Berg DD, Brea EJ, Deutsch AJ, Kidia KK, Thurber EG, Polsky SB, Yeh T, Duskin JA, Holliday AM, Gay EB, Fredenburgh LE. A Case of COVID-19 and Pneumocystis jirovecii Coinfection. Am J Respir Crit Care Med. 2020 Jul 1;202(1):136-138. doi: 10.1164/rccm.202003-0766LE. PMID: 32412848; PMCID: PMC7328312.
- Neff RT, Jindal RM, Yoo DY, Hurst FP, Agodoa LY, Abbott KC. Analysis of USRDS: incidence and risk factors for Pneumocystis jiroveci pneumonia. Transplantation. 2009 Jul 15;88(1):135-41. doi: 10.1097/TP.0b013e3181aad256. PMID: 19584693.
- Avino LJ, Naylor SM, Roecker AM. Pneumocystis jirovecii Pneumonia in the Non-HIV-Infected Population. Ann Pharmacother. 2016 Aug;50(8):673-9. doi: 10.1177/1060028016650107. Epub 2016 May 30. PMID: 27242349.
- Guaraldi G, Meschiari M, Cozzi-Lepri A, Milic J, Tonelli R, Menozzi M, Franceschini E, Cuomo G, Orlando G, Borghi V, Santoro A, Di Gaetano M, Puzzolante C, Carli F, Bedini A, Corradi L, Fantini R, Castaniere I, Tabbì L, Girardis M, Tedeschi S, Giannella M, Bartoletti M, Pascale R, Dolci G, Brugioni L, Pietrangelo A, Cossarizza A, Pea F, Clini E, Salvarani C, Massari M, Viale PL, Mussini C. Tocilizumab in patients with severe COVID-19: a retrospective cohort study. Lancet Rheumatol. 2020 Aug;2(8):e474-e484. doi: 10.1016/S2665-9913(20)30173-9. Epub 2020 Jun 24. Erratum in: Lancet Rheumatol. 2020 Oct;2(10):e591. PMID: 32835257; PMCID: PMC7314456.
- Luo P, Liu Y, Qiu L, Liu X, Liu D, Li J. Tocilizumab treatment in COVID-19: A single center experience. J Med Virol. 2020 Jul;92(7):814-818. doi: 10.1002/jmv.25801. Epub 2020 Apr 15. PMID: 32253759; PMCID: PMC7262125.
- Zain Mushtaq M, Bin Zafar Mahmood S, Jamil B, Aziz A, Ali SA. Outcome of COVID-19 patients with use of Tocilizumab: A single center experience. Int Immunopharmacol. 2020 Nov;88:106926. doi: 10.1016/j.intimp.2020.106926. Epub 2020 Aug 28. PMID: 32889236; PMCID: PMC7455148.
- Scott LJ. Tocilizumab: A Review in Rheumatoid Arthritis. Drugs. 2017 Nov;77(17):1865-1879. doi: 10.1007/s40265-017-0829-7. Erratum in: Drugs. 2017 Dec 19;: PMID: 29094311; PMCID: PMC5736769.
- Kameda H, Tokuda H, Sakai F, Johkoh T, Mori S, Yoshida Y, Takayanagi N, Taki H, Hasegawa Y, Hatta K, Yamanaka H, Dohi M, Hashimoto S, Yamada H, Kawai S, Takeuchi T, Tateda K, Goto H. Clinical and radiological features of acute-onset diffuse interstitial lung diseases in patients with rheumatoid arthritis receiving treatment with biological agents: importance of Pneumocystis pneumonia in Japan revealed by a multicenter study. Intern Med. 2011;50(4):305-13. doi: 10.2169/internalmedicine.50.4508. Epub 2011 Feb 15. PMID: 21325762.
- Schiff MH, Kremer JM, Jahreis A, Vernon E, Isaacs JD, van Vollenhoven RF. Integrated safety in tocilizumab clinical trials. Arthritis Res Ther. 2011;13(5):R141. doi: 10.1186/ar3455. Epub 2011 Sep 1. PMID: 21884601; PMCID: PMC3308069.
Content Alerts
SignUp to our
Content alerts.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.