> Medicine. 2020 September 18;1(5):156-159. doi: 10.37871/jbres1136.
-
Subject area(s):
- Pulmonology
- Hypertension
- Cardiovascular Diseases
Patient Demographics Associated with ARDS Incidence, Hospital Length of Stay and Mortality
Tim W Gilmore* and Clifton F Frilot
- ARDS
- ARDS incidence
- ARDS-related demographics
- ARDS-related mortality
Methods: A retrospective analysis of Electronic Health Record (EHR) data identified 595 adult subjects that received an ARDS diagnosis: ICD-9: 518.82, ICD-10: J96.00 or J80 annotation. The analysis spanned a 30-month period, evaluating subjects by age, gender, race, BMI, LOS, and mortality.
Results: The majority of subjects were admitted through the Emergency Department (408: 68.6%) and were followed by Internal Medicine (137: 23%) or Trauma service (117: 19.7%). A significant portion of subjects expired (130: 21.8%), but a majority were discharged to home care (212: 35.6%). A binomial logistic regression was performed to identify whether a prevalence or risk ratio could be identified between subject demographics and either LOS or mortality. LOS in days was associated with an increased likelihood of mortality (1.055), and age at admission was associated with a reduction in the likelihood of mortality (0.986).
Conclusions: No statistically significant predictor of mortality was identified among subject demographic variables. The findings did suggest that mortality in subjects was higher with longer hospital LOS, lower overall in younger subjects, and inversely related to BMI.
Acute Respiratory Distress Syndrome (ARDS) is a common finding among a broad spectrum of patients in both pediatric and adult populations [1]. This clinical condition manifests as a result of various pulmonary and extrapulmonary disease [2] with a high prevalence of mechanical ventilation requirement [1,3] and common persistent negative effects in survivors [4]. To date, ARDS-related mortality remains high [5] with the associated clinical course resulting in a prolonged hospital Length of Stay (LOS) including multiple days spent in the Intensive Care Unit (ICU) [3]. Certain ARDS phenotypes and endotypes have been identified but the current understanding of causal determinants remains incomplete [6,7].
ARDS remains a challenge to treat and accounts for 1 of 10 ICU patients and roughly 40% of hospital-related deaths [8]. Risk factors such as transfusion, trauma, and advanced age have been associated with an increase in ARDS-related death [9,10]. Although various ARDS-predisposing conditions have long been established, there is high variability in ventilator management strategies during ARDS treatment which make outcomes difficult to correlate with demographics [8,11].
Emerging research has suggested that higher BMI is associated with increased LOS but decreased mortality for patients with ARDS [12,13]. However, recent findings indicate that COVID-19 related deaths are more prevalent in patients with higher BMI [14] and that obesity should be considered an independent risk factor for mortality in patients with COVID-19 [15]. Obesity has been also linked to increased incidence of hospital admission in younger patients [16].
Studies reveal a significant portion of ARDS survivors require post-discharge follow-up hospitalization and other chronic treatments [17] and have sought to predict whether certain risk factors can be associated with ARDS development and higher mortality. Certain studies have suggested that higher ARDS associated mortality rates are observed in older subjects of non-white and non-black race [18] and that ARDS management and outcomes may vary according to gender [11]. It remains to be established whether a strong association exists between ARDS patient demographic characteristics, hospital LOS and overall ARDS-related mortality [8]. This study sought to identify whether certain associations exist between particular demographics, ARDS incidence, LOS, and ARDS-related mortality and if a known variable placed a patient at higher risk for ARDS development, increased LOS, or mortality.
After obtaining Institutional Review Board approval, a retrospective analysis of the Electronic Health Record (EHR) was performed in July 2018 at a large academic medical center to identify all adult patients that received an ARDS diagnosis. All adult subjects that were assigned an International Classification of Diseases (ICD) code ICD-9: 518.82 or ICD-10: J96.00 or J80 EHR denotation were included. Although of interest, there was no evaluation of the nuances of decision-making related to the ICU care subjects received. The analysis spanned a 30-month period, identifying 595 total subjects among all available ICUs. All raw data was compiled into a database where available variables for age, gender, race, BMI, LOS, and in-hospital mortality were evaluated.
Data analysis was performed by Statistical Package for Social Sciences (SPSS) version 24 and Microsoft Excel. Descriptive statistics are reported in table 1. The majority of subjects were male (335/592: 56.3%), admitted through the Emergency Department (408/595; 68.6%), Medical ICU (51/595; 8.6%), and Neuro ICU (37/595; 6.2%), and were followed by Internal Medicine (137/595; 23%), Trauma (117/595; 19.7%), or Medical ICU service (95/595; 16%). A significant portion of subjects expired (130/595; 21.8%), although mortality rate for this study was lower than overall ARDS-related mortality trends of recent years [5]. The average LOS was 13.4 days with most survivors discharged to homecare (212/595; 35.6%).
A binomial logistic regression was performed to identify whether a prevalence or risk ratio could be identified between subject demographics and either LOS or mortality. The logistic regression model was statistically significant (Χ2(6) = 55.139, p < .001) and explained 13.9% (Nagelkerke R2) of the variance in mortality outcome, correctly classifying 77.9% of the cases. LOS in days was associated with an increased likelihood of mortality (1.055); however, age at admission was associated with a reduction in likelihood of mortality (0.986).
No statistically significant predictor of mortality was identified among subject demographic variables. The findings did suggest that mortality in subjects with ARDS is higher with longer hospital length of stay. Mortality rate was lower in younger subjects and found inversely related to BMI.
| Table 1: ARDS Subject Demographics. | ||||
| n = 592 | ARDS Incidence | LOS (days) M (SD) 13.41 (14.02) |
Mortality (n = 130) |
|
| Age (years) (n = 592) M (Range) 56.19 (18-96) |
18-30 | 57 (9.6%) | 15.98, (16.8) | 10/57(17.5%) |
| 31-50 | 132 (22.3%) | 15.29 (18.4) | 27/131 (20.6%) | |
| 51-70 | 275 (46.5%) | 12.56 (12.5) | 60/292 (20.5%) | |
| > 70 | 127 (21.4%) | 12.10 (9.2) | 33/112 (29.4%) | |
| Gender (n = 592) |
Male | 335 (56.5%) | 14.4 (14.4) | 77/335 (22.9%) |
| Female | 257 (43.4%) | 12.0 (12.9) | 53/257 (20.6%) | |
| Race (n = 592) |
Black | 313 (52.6%) | 12.4 (14.1) | 63/269 (23.4%) |
| White | 269 (45.2%) | 14.4 (13.5) | 65/313 (20.7%) | |
| Other | 10 (1.7%) | 13.2 (11.1) | 2/10 (20%) | |
| BMI (n = 579) M (SD) 28.7 (8.9) |
< 18.5 | 41 (7%) | 14.02 (13.5) | 11/39 (28.2%) |
| 18.5 – 24.9 | 181 (31.2%) | 13.15 (13.0) | 42/155 (27.1%) | |
| 25-29.9 | 149 (25.7%) | 13.58 (14.5) | 34/163 (20.8%) | |
| > 30 | 208 (35.9%) | 13.41 (14.3) | 39/208 (18.7%) | |
This study sought to identify associations between ARDS patient demographics, hospital LOS and mortality in subjects from a single center within a fixed time frame. It was not possible to verify the exact criteria used by each provider that determined the ARDS diagnosis, and although ARDS diagnosis for each subject was input sometime during the visit, it was not possible to identify the exact time of diagnosis. A patient’s LOS may have been interrupted or altered due to various protocol unrelated to clinical care (i.e. transfer due to insurance/reimbursement criteria). Certain confounding variables were not necessarily addressed such as pre-existing conditions and other comorbidities. Although of interest, mechanical ventilation strategies and settings were not evaluated.
Only the most prevalent categories were reported based upon the initial EHR extraction report, and categorical variables reported as available. The area to which subjects were admitted, cared for, and discharged was highly variable. Although of interest, the particular ICU of care was not correlated to ARDS diagnosis or management as actual ARDS diagnosis date was difficult to identify.
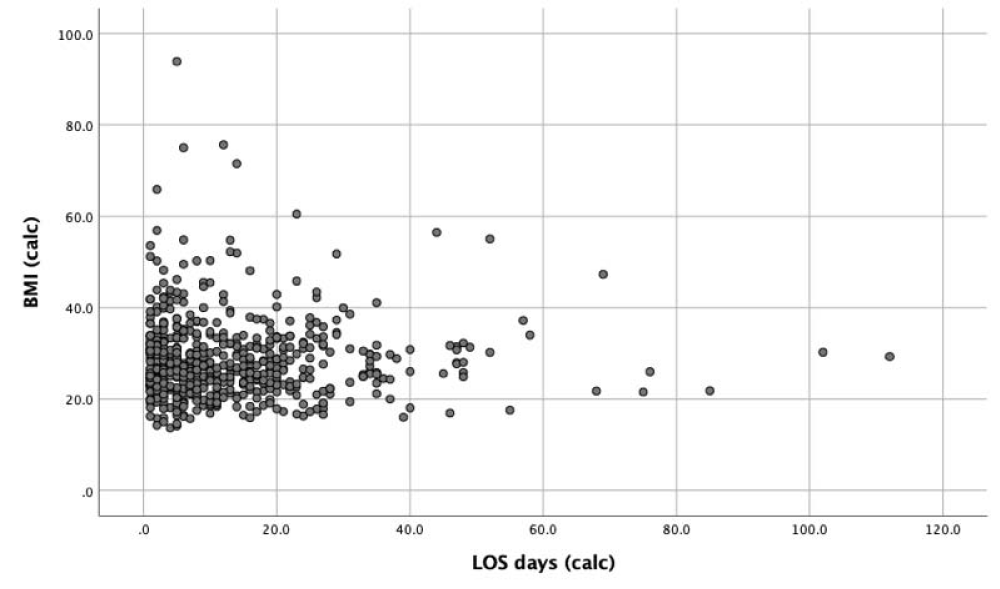
An emerging body of research suggests that a lower BMI may be independently associated with overall increased risk of mortality, but ICU patients with higher BMI may have greater survival rates [12,19]. Our study did not identify BMI as a statistically significant predictor of mortality. However, BMI was inversely related to mortality rate with lower BMI associated with highest mortality and higher BMI associated with lowest mortality. Furthermore, our study suggested that LOS was greater in subjects with a higher BMI (Figure 1) although these subjects had a lower mortality rate.
The so-called "obesity paradox" implies that higher BMI is an independent risk factor for ARDS development, but better outcomes are observed in patients with higher BMI compared to normal BMI [12]. It is well known that obesity is a pro-inflammatory condition with potential negative impact on lung function due to cytokine mediation [20], but there remains inquiry surrounding whether higher BMI may positively impact the long-term outcomes in patients with ARDS. Future studies are needed to further elucidate particular patient demographics linked to ARDS incidence, Hospital Length of Stay, and Mortality.
There is ongoing research to evaluate the implications of obesity within the context of COVID-19. A systematic review by Yang, et al. [21] identified a greater severity of COVID-19 in patients with higher BMI, and a recent systematic review by Popkin, et al. [22] revealed that obesity placed patients at higher risk for development of COVID-19 with increased hospitalization, ICU admission, and overall mortality. As the COVID-19 pandemic persists, ARDS and COVID-19 induced respiratory failure may be difficult to differentiate and the clinical management strategies for each variable [23]. There is a possibility that the obesity paradox is not observed in patients with COVID-19, but research is ongoing.
- Ware LB, Matthay MA. The acute respiratory distress syndrome. N Engl J Med. 2000; 342: 1334-1349. DOI: 10.1056/NEJM200005043421806. https://bit.ly/32zJCOl
- Gattinoni L, Pelosi P, Suter PM, Pedoto A, Vercesi P, Lissoni A. Acute respiratory distress syndrome caused by pulmonary and extrapulmonary disease. Different syndromes? Am J Respir Crit Care Med. 1998 Jul;158(1):3-11. doi: 10.1164/ajrccm.158.1.9708031. PMID: 9655699.
- Bellani G, Laffey JG, Pham T, Fan E, Brochard L, Esteban A, Gattinoni L, van Haren F, Larsson A, McAuley DF, Ranieri M, Rubenfeld G, Thompson BT, Wrigge H, Slutsky AS, Pesenti A; LUNG SAFE Investigators; ESICM Trials Group. Epidemiology, Patterns of Care, and Mortality for Patients With Acute Respiratory Distress Syndrome in Intensive Care Units in 50 Countries. JAMA. 2016 Feb 23;315(8):788-800. doi: 10.1001/jama.2016.0291. Erratum in: JAMA. 2016 Jul 19;316(3):350. Erratum in: JAMA. 2016 Jul 19;316(3):350. PMID: 26903337.
- Herridge MS, Tansey CM, Matté A, Tomlinson G, Diaz-Granados N, Cooper A, Guest CB, Mazer CD, Mehta S, Stewart TE, Kudlow P, Cook D, Slutsky AS, Cheung AM; Canadian Critical Care Trials Group. Functional disability 5 years after acute respiratory distress syndrome. N Engl J Med. 2011 Apr 7;364(14):1293-304. doi: 10.1056/NEJMoa1011802. PMID: 21470008.
- Máca J, Jor O, Holub M, Sklienka P, Burša F, Burda M, Janout V, Ševčík P. Past and Present ARDS Mortality Rates: A Systematic Review. Respir Care. 2017 Jan;62(1):113-122. doi: 10.4187/respcare.04716. Epub 2016 Nov 1. PMID: 27803355.
- Pham T, Rubenfeld GD. Fifty Years of Research in ARDS. The Epidemiology of Acute Respiratory Distress Syndrome. A 50th Birthday Review. Am J Respir Crit Care Med. 2017 Apr 1;195(7):860-870. doi: 10.1164/rccm.201609-1773CP. PMID: 28157386.
- Shankar-Hari M, McAuley DF. Acute Respiratory Distress Syndrome Phenotypes and Identifying Treatable Traits. The Dawn of Personalized Medicine for ARDS. Am J Respir Crit Care Med. 2017 Feb 1;195(3):280-281. doi: 10.1164/rccm.201608-1729ED. PMID: 28145757.
- McNicholas BA, Rooney GM, Laffey JG. Lessons to learn from epidemiologic studies in ARDS. Curr Opin Crit Care. 2018 Feb;24(1):41-48. doi: 10.1097/MCC.0000000000000473. PMID: 29135617.
- Eworuke E, Major JM, Gilbert McClain LI. National incidence rates for Acute Respiratory Distress Syndrome (ARDS) and ARDS cause-specific factors in the United States (2006-2014). J Crit Care. 2018 Oct;47:192-197. doi: 10.1016/j.jcrc.2018.07.002. Epub 2018 Jul 10. PMID: 30015289.
- Rubenfeld GD, Caldwell E, Peabody E, Weaver J, Martin DP, Neff M, Stern EJ, Hudson LD. Incidence and outcomes of acute lung injury. N Engl J Med. 2005 Oct 20;353(16):1685-93. doi: 10.1056/NEJMoa050333. PMID: 16236739.
- McNicholas BA, Madotto F, Pham T, Rezoagli E, Masterson CH, Horie S, Bellani G, Brochard L, Laffey JG; LUNG SAFE Investigators and the ESICM Trials Group. Demographics, management and outcome of females and males with acute respiratory distress syndrome in the LUNG SAFE prospective cohort study. Eur Respir J. 2019 Oct 17;54(4):1900609. doi: 10.1183/13993003.00609-2019. PMID: 31346004.
- Gong MN, Bajwa EK, Thompson BT, Christiani DC. Body mass index is associated with the development of acute respiratory distress syndrome. Thorax. 2010 Jan;65(1):44-50. doi: 10.1136/thx.2009.117572. Epub 2009 Sep 21. PMID: 19770169; PMCID: PMC3090260.
- Ni YN, Luo J, Yu H, Wang YW, Hu YH, Liu D, Liang BM, Liang ZA. Can body mass index predict clinical outcomes for patients with acute lung injury/acute respiratory distress syndrome? A meta-analysis. Crit Care. 2017 Feb 22;21(1):36. doi: 10.1186/s13054-017-1615-3. PMID: 28222804; PMCID: PMC5320793.
- Sattar N, Ho FK, Gill JM, Ghouri N, Gray SR, Celis-Morales CA, Katikireddi SV, Berry C, Pell JP, McMurray JJ, Welsh P. BMI and future risk for COVID-19 infection and death across sex, age and ethnicity: Preliminary findings from UK biobank. Diabetes Metab Syndr. 2020 Sep-Oct;14(5):1149-1151. doi: 10.1016/j.dsx.2020.06.060. Epub 2020 Jun 30. PMID: 32668401; PMCID: PMC7326434.
- Caci G, Albini A, Malerba M, Noonan DM, Pochetti P, Polosa R. COVID-19 and Obesity: Dangerous Liaisons. J Clin Med. 2020 Aug 4;9(8):2511. doi: 10.3390/jcm9082511. PMID: 32759719; PMCID: PMC7465218.
- Lighter J, Phillips M, Hochman S, Sterling S, Johnson D, Francois F, Stachel A. Obesity in Patients Younger Than 60 Years Is a Risk Factor for COVID-19 Hospital Admission. Clin Infect Dis. 2020 Jul 28;71(15):896-897. doi: 10.1093/cid/ciaa415. PMID: 32271368; PMCID: PMC7184372.
- Ruhl AP, Huang M, Colantuoni E, Karmarkar T, Dinglas VD, Hopkins RO, Needham DM; With the National Institutes of Health, National Heart, Lung, and Blood Institute Acute Respiratory Distress Syndrome Network. Healthcare utilization and costs in ARDS survivors: a 1-year longitudinal national US multicenter study. Intensive Care Med. 2017 Jul;43(7):980-991. doi: 10.1007/s00134-017-4827-8. Epub 2017 May 26. PMID: 28550403.
- El-Haddad H, Jang H, Chen W, Haider S, Soubani AO. The effect of demographics and patient location on the outcome of patients with acute respiratory distress syndrome. Ann Thorac Med. 2017 Jan-Mar;12(1):17-24. doi: 10.4103/1817-1737.197767. PMID: 28197217; PMCID: PMC5264167.
- Sakr Y, Alhussami I, Nanchal R, Wunderink RG, Pellis T, Wittebole X, Martin-Loeches I, François B, Leone M, Vincent JL; Intensive Care Over Nations Investigators. Being Overweight Is Associated With Greater Survival in ICU Patients: Results From the Intensive Care Over Nations Audit. Crit Care Med. 2015 Dec;43(12):2623-32. doi: 10.1097/CCM.0000000000001310. PMID: 26427591.
- Zhi G, Xin W, Ying W, Guohong X, Shuying L. "Obesity Paradox" in Acute Respiratory Distress Syndrome: Asystematic Review and Meta-Analysis. PLoS One. 2016 Sep 29;11(9):e0163677. doi: 10.1371/journal.pone.0163677. PMID: 27684705; PMCID: PMC5042414.
- Yang J, Hu J, Zhu C. Obesity aggravates COVID-19: a systematic review and meta-analysis. J Med Virol. 2020 Jun 30:10.1002/jmv.26237. doi: 10.1002/jmv.26237. Epub ahead of print. PMID: 32603481; PMCID: PMC7361606.
- Popkin BM, Du S, Green WD, Beck MA, Algaith T, Herbst CH, Alsukait RF, Alluhidan M, Alazemi N, Shekar M. Individuals with obesity and COVID-19: A global perspective on the epidemiology and biological relationships. Obes Rev. 2020 Aug 26:10.1111/obr.13128. doi: 10.1111/obr.13128. Epub ahead of print. PMID: 32845580; PMCID: PMC7461480.
- Grieco DL, Bongiovanni F, Chen L, Menga LS, Cutuli SL, Pintaudi G, Carelli S, Michi T, Torrini F, Lombardi G, Anzellotti GM, De Pascale G, Urbani A, Bocci MG, Tanzarella ES, Bello G, Dell’Anna AM, Maggiore SM, Brochard L, Antonelli M. Respiratory physiology of COVID-19-induced respiratory failure compared to ARDS of other etiologies. Crit Care. 2020 Aug 28;24(1):529. doi: 10.1186/s13054-020-03253-2. PMID: 32859264; PMCID: PMC7453378.
Content Alerts
SignUp to our
Content alerts.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.